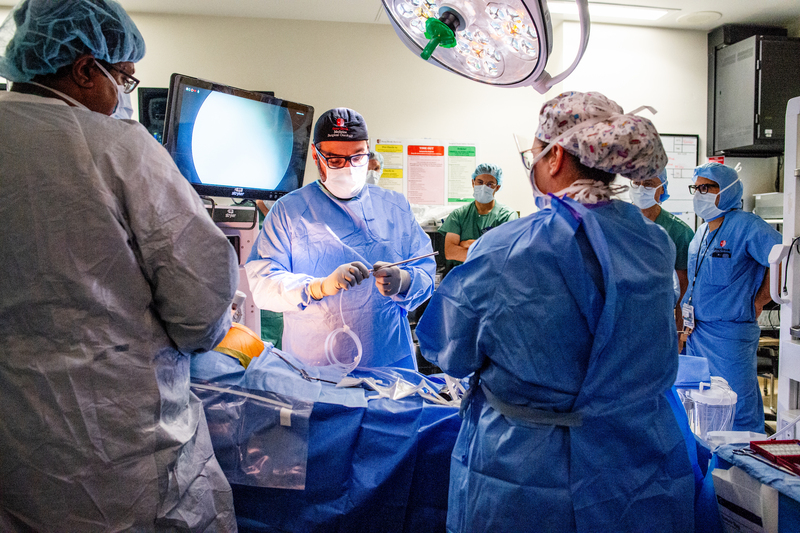
Stony Brook Medicine (SBM) continues to demonstrate its national leadership role in implementing novel and innovative surgical techniques to benefit patients with cancer. On September 21-22, 2023, SBM's Department of Surgery and Stony Brook Cancer Center presented the first Pressurized Intraperitoneal Aerosol Chemotherapy (PIPAC) Workshop for surgeons held in the northeastern U.S., and the second ever workshop of this kind in the US. The PIPAC procedure uses pressurized intraperitoneal aerosol chemotherapy during cancer surgery. The workshop, held at Stony Brook University Hospital, included a case observation, which was the first performed outside of research studies in the U.S.
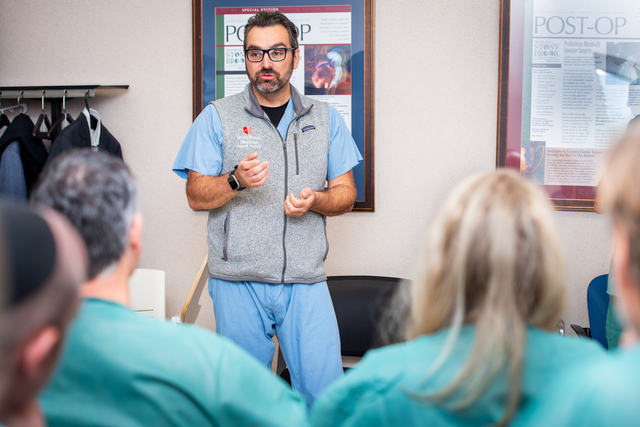
The two-day workshop, which used the current commercially available equipment, was hosted by Georgios V. Georgakis, MD, PhD, FACS, surgical oncologist and Associate Professor of Surgery at SBM, and Professor Marc Pocard from the Université Paris Cité, INSERM; Hepato-Biliary-Pancreatic Gastrointestinal, Surgery and Liver Transplantation, Pitié Salpêtrière Hospital in France. Twelve cancer surgeons from across the U.S., and the country of Colombia, attended classroom sessions, observed the PIPAC procedure as it was performed on a patient, and were tested on the workshop content to earn a certificate. The case observation was of a 68-year-old male patient with disseminated intraperitoneal cancer. Attendee response to the workshop was extremely positive and enthusiastic, as demonstrated by a quick survey at the end of the workshop.

Novel Treatment for Abdominal Cancers
The PIPAC procedure has been used as a treatment option outside of the US for a number of years. The first PIPAC procedure was performed in November 2011 in Germany by Dr. Marc Reymond. Professor Marc Pocard has performed this procedure numerous times in Paris and across Europe. PIPAC is generally used for end-stage peritoneal carcinomatosis, stomach cancer, ovarian cancer, colorectal cancer and other tumors that have been disseminated in the peritoneal cavity (e.g., appendix cancer). This innovative method of delivering chemotherapy to the abdomen via a pressurizing nebulizer is considered a safe option for patients with terminal disease and no other effective means of treatment because it is less toxic, less invasive and presents fewer complications for the patient.

The current common treatments for these types of cancers include:
- Systemic chemotherapy - An injection or infusion of chemotherapy into a vein (the chemotherapy then travels throughout the body in the bloodstream)
- Cytoreductive surgery and HIPEC (Hyperthermic Intraperitoneal Chemotherapy) - An option for certain eligible patients, which is more invasive (as it requires a larger incision) and requires a much longer hospital stay
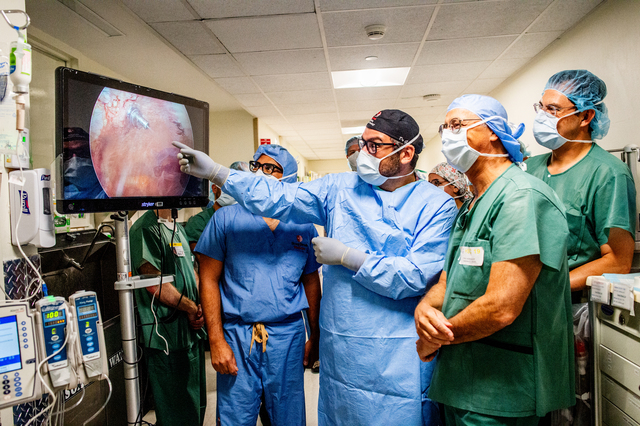
PIPAC offers an alternate treatment option for patients who cannot tolerate HIPEC or as an adjunct in traditional chemotherapy. It is also an ideal treatment for patients with malignant ascites, which is a condition where malignant cells shed in the peritoneal cavity and cause fluid to accumulate. While this is extremely difficult to treat with intravenous chemotherapy, PIPAC offers both a palliative and a therapeutic solution, with draining the excess fluid and treating the very same cancer cells that cause it.

Technology Innovation Allows for Lower Morbidity and Wider Application to More Patients
PIPAC uses a wand-like device attached to high-pressure tubing that is connected to a standard injector pump. After the wand is inserted laparoscopically, through a small incision in the abdomen, and is positioned for optimal chemotherapy distribution in the targeted area, the device aerosolizes the chemotherapy into a fine mist (similar to asthma medication delivered via a nebulizer). This process allows for lower dosage intraperitoneal chemotherapy, with a wider distribution and a deeper penetration into the tissue.

The lower toxicity and systemic concentration, smaller incision and reduced hospital stay (usually one night) position PIPAC as a safe method for delivering chemotherapy drugs in patients with late-stage cancer. Most patients will not have to stop their standard chemotherapy regimen, but some may have to take a very short break. PIPAC may also be used more than once, over a course of sessions, and is done under general anesthesia and generally takes about thirty minutes. Studies show that most patients tolerate this procedure well, experience fewer side effects and that complications are rare. PIPAC has been shown to improve a patient's quality of life and potentially extend life expectancy.
Dr. Georgakis has spearheaded the drive to bring the PIPAC procedure to his colleagues throughout the U.S. He was inspired to learn the procedure from treating his patients who could benefit from this type of procedure.
Additional PIPAC training workshops at Stony Brook University Hospital are planned for early 2024. For more information, please call or email Luis Ehrman in Stony Brook's Division of Surgical Oncology at (631)444-8086 and Luis.Ehrman1@stonybrookmedicine.edu.

