Division of Orthopedic and Plastics Anesthesia
- Introduction
- Pre-Operative Services (POS)
- The Day before Surgery
- The Day of Surgery in the Pre Surgical Unit
- Types of Anesthesia
- Frequently Asked Questions (FAQ)
- Stony Brook Department of Orthopedics | About Your Orthopedic Surgery
- Download our Brochure
Introduction
 The Division of Orthopedic & Plastics Anesthesia welcomes you to Stony Brook University Hospital. The team members of our Division work closely with the Acute Pain Service (APS) and the orthopedic surgeons to assure that your in-hospital experience is as pleasant as possible. Our Division places patient safety, your comfort, and your satisfaction as its number one clinical priority.
The Division of Orthopedic & Plastics Anesthesia welcomes you to Stony Brook University Hospital. The team members of our Division work closely with the Acute Pain Service (APS) and the orthopedic surgeons to assure that your in-hospital experience is as pleasant as possible. Our Division places patient safety, your comfort, and your satisfaction as its number one clinical priority.This is a brief narrative outlining the typical anesthesia-related encounters and procedures a given patient will experience when choosing to have a total joint replacement at our Hospital. However, there are often various medical issues which may require us to modify our practice to optimize your individual care. Please do not hesitate to contact us by telephone or visit our website for additional information.
Pre-Operative Services (POS)
Within 30-days prior to your surgery, you will be asked to undergo a pre-operative evaluation at the POS Center within SBUH. The pre-op evaluation will help us determine your general health condition and your overall risk of surgery. At the POS visit, you will have a complete history and a physical examination. You will also have any indicated laboratory testing which may include some or all of the following: blood tests, EKG, x-rays. An anesthesiologist will discuss the anesthesia plan and answer any related questions. Depending on your other medical conditions, further evaluation or testing may be requested.
Please bring a list of all your medications and your reading glasses to this appointment. On the day of the POS visit you may eat and drink as usual.
The Day before Surgery
You should expect a telephone call from the Acute Pain Service team regarding your choice of anesthesia/ analgesia. Any additional questions or concerns that you may have can also be discussed at this time.
The Day of Surgery in the Pre Surgical Unit
After the check-in process is completed, you will meet with an anesthesiologist from the Acute Pain Service team who will again explain your options for anesthesia and pain management (analgesia), and its associated risks and benefits. There are multiple types of anesthesia which can be used in the setting of a total joint replacement, and sometimes a combination of the different types may be beneficial. At SBUH, we prefer ‘regional’ anesthesia for both the surgery and postoperative pain control. If you are scheduled to have total knee replacement, you will be given a femoral nerve block to control the pain after the surgery as well as spinal anesthesia.
Types of Anesthesia
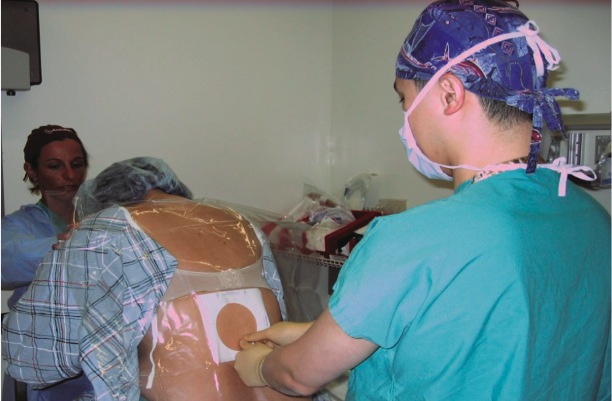
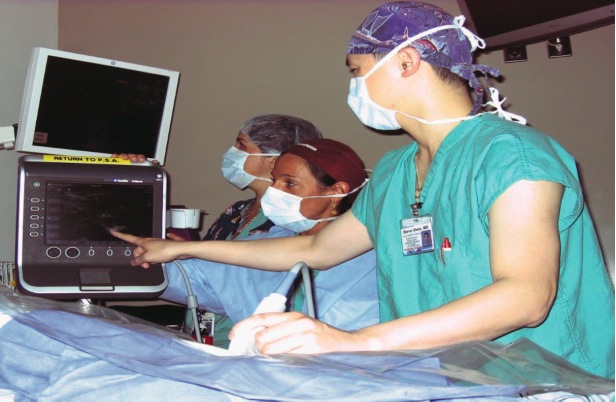 Femoral Nerve Block
Femoral Nerve BlockAt SBUH, a femoral nerve block has been an effective technique for pain control immediately after surgery in patients undergoing total knee replacement.
The nerve block placement begins with sedation, and once you are adequately sedated, the anesthesiologist will clean off your groin on the side of the planned surgery.
Next, the anesthesiologist will use a thin needle to locate the femoral nerve with the help of ultrasound visualization. We also employ a very low amount of electrical current through the needle to accurately locate the nerve. Some patients recall their leg twitching automatically. This is the response your anesthesiologist is trying to obtain.
Once the nerve is located, your anesthesiologist will inject a long-acting local anesthetic to numb the nerve and with it, the front of your knee. The numbness in the front of your knee lasts an average of sixteen hours.
The block alone is usually not enough pain relief, so patients will also need narcotics in addition to the femoral nerve block to help ease the pain.
Spinal Anesthesia
Spinal anesthesia is a safe and effective means of anesthesia during surgery, and this is the method most commonly used for most joint replacement surgeries. It involves an injection of medication (usually a local anesthetic) into the lower portion of the spine which numbs and paralyzes the lower half of the body (usually below the navel).
Most spinal injections are quick and delivered with a numbing anesthetic (lidocaine) around the skin. The injection is usually made at the lower end of the spine below where the spinal cord itself ends. Doing the injection this way decreases the risk of any sort of spinal cord injury.
Combined Epidural-Spinal Anesthesia
The Combined Epidural-Spinal technique is the preferred anesthesia method for total hip replacement. This technique is performed once you have received some sedation through your I.V. Patients often have no recollection of undergoing an epidural-spinal.
Once you are sedated, your anesthesiologist will sit you upright for the procedure and your back will be cleaned. A small amount of local anesthetic is used to numb your skin at the site of the procedure. Your anesthesiologist will then insert an epidural needle into the epidural space. Once in the correct space, a smaller spinal needle will be inserted through the epidural needle to reach the spinal fluid.
Once the needle is in place, an appropriate amount of local anesthetic is injected. A small plastic tube (catheter) is then inserted into the epidural space and all needles are removed. The plastic tubing will stay for twenty-four hours after the surgery in order to deliver the local anesthetics, which keep the hip pain-free.
General Anesthesia
General anesthesia refers to the patient "going completely under," typically requiring placement of a breathing tube and having the ventilator machine breathe for them while they are asleep. The term "general" is used because this type of anesthesia affects the entire body, including loss of consciousness. For most patients, the last thing they remember is the medication going into the I.V. The breathing tube is typically inserted after sedation and is removed before awakening, so generally, you do not remember the tube (although you might have a sore throat afterwards).
General anesthesia can be used for many hours if necessary, and it is needed for very large and complex surgeries. However, it is more likely to produce nausea and vomiting after surgery, and most patients can feel drowsy or weak for several days after the anesthesia (like a hangover).
 Frequently Asked Questions (FAQ)
Frequently Asked Questions (FAQ)
What is regional anesthesia?
The term regional anesthesia refers to anesthesia which affects or numbs only part of the body (e.g. leg or arm). We employ femoral nerve blockade or spinal and/or epidural procedures for this purpose. These procedures are described in detail in this patient guide.
Do I have to be awake during the regional anesthesia procedures?
Sedation is a significant part of a smooth surgical experience. We provide medications that will relieve your anxiety and pain before the performance of the blocks so that usually you will be unaware of having experienced the regional anesthetic procedure.
Will I be asleep during the surgical procedure?
The level of sedation experienced varies. Some patients may remember a lot, and some may not remember anything at all until they wake up in the recovery room. It is the decision of the anesthesiologist as to how to manage your level of sedation in order to provide you with as smooth and safe an experience as possible.
How will my pain be controlled when I wake up from surgery?
In the Post-Anesthesia Care Unit (PACU), after the spinal wears off, the femoral nerve or epidural catheter infusion will be started by an anesthesiologist for post-operative pain control. In addition, other medications may be used to keep your pain controlled. You will not leave the PACU until your pain and other care is well-controlled. Further, on the orthopedic floor, the Acute Pain team will be checking on you to make sure that your pain is under control. Twenty-four hours later, your local anesthesia catheter is removed and your pain will be controlled with oral medication.
