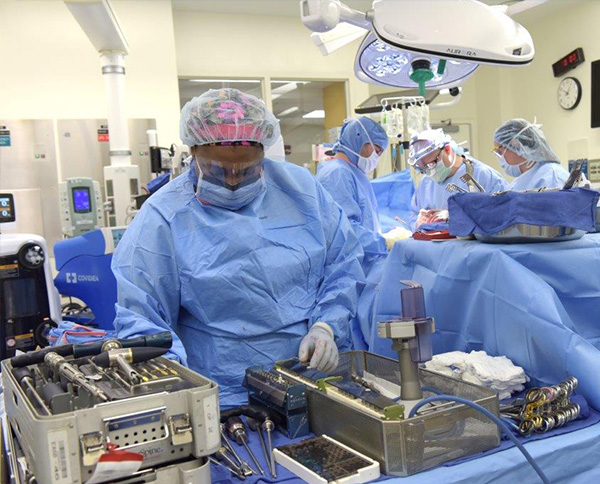
 A large quantity of any hospital’s environmental footprint is produced by its operating rooms. Studies estimate that between 20-30 percent of the total waste volume generated by a hospital comes from ORs. Operating rooms are one of the largest users of supplies within a hospital. Surgical kits are often wrapped with plastic after sterilization and boxed, and many instruments are individually wrapped. This packaging ends up in the waste stream. Halogenated anesthetic agents are released into the environment during use and present significant climate harm potential. To address these issues, SBUH continues to explore environmentally sustainable ways of managing operating room.
A large quantity of any hospital’s environmental footprint is produced by its operating rooms. Studies estimate that between 20-30 percent of the total waste volume generated by a hospital comes from ORs. Operating rooms are one of the largest users of supplies within a hospital. Surgical kits are often wrapped with plastic after sterilization and boxed, and many instruments are individually wrapped. This packaging ends up in the waste stream. Halogenated anesthetic agents are released into the environment during use and present significant climate harm potential. To address these issues, SBUH continues to explore environmentally sustainable ways of managing operating room.
Goals for 2026:
- OR setbacks: Complete design this year
- Remove anesthesia machine from ACP endo
- Continue reviewing OR material packets to reduce waste, identifying items for removal that are not used
- Consideration of feasibility of central nitrous system removal
Recent Highlights:
The Department of Anesthesia made a huge leap forward on their commitment to sustainability this past. To recognize these efforts a manuscript was accepted and published by Faculty leadership. We continue to mentor students interested in sustainability and this year worked with an undergraduate student in the Department to further our efforts and cross-campus integration.
Stony Brook University Hospital is mid-construction on an off-site surgical center that will expand access to ambulatory operating rooms and better meet the needs of Suffolk County residents. There will be a total of four ORs, with the first two expected to open in the Fall of 2026. These suites incorporate multiple sustainability features. It is anticipated that no (or very small quantities of) desflurane and nitrous oxide will be used. The suites will have programmed setbacks for lighting and HVAC systems. Surgical lighting will all be LED. Surgical smoke evacuation systems will be employed to reduce staff exposures and impacts. The outpatient facility will customize procedure packs and preference will be given to reusable surgical items, when clinically and financially appropriate. Medical waste will be segregated at each step of the surgical process and disposed of appropriately. Reusable sterilization trays will be used to reduce blue wrap, and we will educate staff to collect single-use items for reprocessing when appropriate. We anticipate 1500 procedures will be performed in the first year of operation.
Inhaled anesthetic gases are a significant source of greenhouse gas emissions from a hospital. SBUH has worked to reduce the total amount used and has specifically focused on desflurane. Desflurane is similar in clinical action to several other drugs but has a much larger environmental impact. Desflurane is still available for use, but only with special arrangements.
Nitrous oxide is also a common inhaled anesthetic gas, of a different category than desflurane. It also negatively impacts the environment and remains very active for an extended period of time. Minimization of nitrous is a goal, and SBUH has seen reductions in its use over time.
Overall, our GHG emissions from Anesthesia per Anesthesia Hour have decreased from 2023 to 2025. We are currently in the lowest quartile in a recent academic medical center cohort.
To increase recycling, efforts are being made to ensure appropriate used OR medical supplies are placed into correct recycling bins. In addition, we encourage the purchase of upcycled medical devices wherever feasible.
Surgical case packs (kits of supplies organized by surgical service are reviewed annually. he annual accounting and reporting process identifies instruments not being used, so we can remove them from the kits and reduce waste. We are working with our primary implant vendors to reduce tray weights and shift to validated containers whenever possible.
Stony Brook University Hospital collects for reprocessing several categories of single use equipment, including air transfer mattresses, EP catheters, and pulse ox sensors. In CY 2025 the collected items exceeded 13,400 items or 1,214 pounds of avoided waste. That is equivalent to 43,379 water bottles and a GHG offset of more than 39 metric tons. We also purchased reprocessed single use devices at a substantial savings with no additional patient risk, further supporting the marketplace. It is anticipated that the program will continue to expand to additional materials, both as a waste diversion to reprocessing and more sustainable purchasing. From the vendor, for CY 2025:
Recent Recognition:
Practice Greenhealth has recognized the work of this group with Greening the OR awards in 2018, 2019, 2020, 2022, and 2024.
Team Leaders:
Ally Silver, Mike DeMasi, Cynthia Jorgensen, and Martha Houlihan
