 KNEE OSTEOARTHRITIS
KNEE OSTEOARTHRITIS
Osteoarthritis, also known as wear-and-tear or degenerative arthritis, is the most common form of the disease, affecting millions of people in the US each year. This condition is most common in older patients whose cartilage has worn down over time, and in athletes who have worn down their cartilage from overuse and repetitive motions.
Patients with osteoarthritis may experience pain, swelling and stiffness within the joint, which tend to worsen as the condition progresses. Your doctor can diagnose this condition after evaluating your symptoms and performing an X-ray examination of the knee. Several other factors should be taken into consideration when diagnosing osteoarthritis, including evaluation of the patient’s spine, nearby joints, posture and gait.
Treatment for osteoarthritis initially focuses on relieving pain and other symptoms, and may include rest, physical therapy, bracing and anti-inflammatory medication. More severe cases of osteoarthritis may require surgery to reposition the bones or replace the joint. Most procedures can be performed through arthroscopy, which significantly reduces bleeding, scarring and recovery times.
KNEE ARTHROSCOPY
Arthroscopy is a minimally invasive procedure that allows doctors to examine tissues inside the knee. It is often performed to confirm a diagnosis made after a physical examination and other imaging tests such as MRI, CT scan or X-rays. During an arthroscopic procedure, a thin fiberoptic light, magnifying lens and tiny television camera are inserted into the knee, allowing your doctor to examine the joint in great detail.
Knee arthroscopy is performed on an outpatient basis under local or general anesthesia, depending on the type and severity of the condition, as well as the patient’s personal preference. During the procedure, the surgeon will insert the arthroscope into the knee through a tiny incision. This instrument is used to identify any damage or abnormalities within the knee, or to confirm the diagnosis of a previous imaging exam.
If damaged areas are detected, they can be repaired during the same procedure by inserting surgical instruments into additional incisions. Knee arthroscopy may include removing torn cartilage, reconstructing torn ligaments, trimming cartilage, removing loose bone or removing other inflamed tissue. Once the repair has been completed, the incisions will be sutured closed and then covered with a bandage.
KNEE REPLACEMENT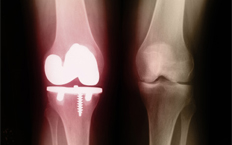 In a total knee replacement, the damaged ends of the bones are removed and replaced with a prosthesis made of metal and plastic. A partial knee replacement for patients with damage on only one side of the joint can delay or prevent a total knee replacement. These artificial parts allow the joint to move smoothly so the patient experiences pain relief and a better quality of life. Knee replacement can also help restore motion to the joint, straighten the leg and improve stability.
In a total knee replacement, the damaged ends of the bones are removed and replaced with a prosthesis made of metal and plastic. A partial knee replacement for patients with damage on only one side of the joint can delay or prevent a total knee replacement. These artificial parts allow the joint to move smoothly so the patient experiences pain relief and a better quality of life. Knee replacement can also help restore motion to the joint, straighten the leg and improve stability.
Recent advances in surgical technology make it possible to perform minimally invasive joint replacements. Traditional knee replacement surgery involves an 8-12 inch incision. Various minimally-invasive techniques allow the joint to be replaced with less cutting and manipulation of muscles, tendons and ligaments around the joint. There are other potential advantages to minimally invasive surgery that help make the surgery safer and allow patients to enjoy a faster and less painful recovery. Our doctors will discuss with you whether you are a candidate for minimally invasive knee replacement surgery.
ACL INJURY
The ACL (anterior cruciate ligament) is one of the most commonly injured ligaments in the knee. Running diagonally through the middle of the joint, the ACL works together with three other ligaments to connect the femur (upper leg bone) to the tibia (lower leg bone). People who play sports that are likely to damage the knee — such as basketball, football, skiing and soccer — are at greatest risk for injuring the ACL. Only about 30% of ACL injuries result from direct contact with another player or object. The rest occur when the athlete decelerates while cutting, pivoting, or sidestepping; lands awkwardly; or plays recklessly. About half of ACL injuries are accompanied by damage to the meniscus, cartilage, bone or other ligaments in the knee.
Signs that you may have injured your ACL include pain, swelling and instability immediately after the injury, followed hours later by greater swelling and pain, limited motion, tenderness and an inability to walk comfortably.
ACL RECONSTRUCTION
ACL reconstruction is usually not performed until several weeks after the injury, when swelling and inflammation have been reduced. The torn ligament is completely removed and replaced with a new ACL. Simply reconnecting the torn ends will not repair the ACL. Part of another ligament, usually from the knee or hamstring, is used to create a graft for the new ACL. Choosing the proper type of graft depends on each patient’s individual condition.
ACL surgery requires a few months for full recovery and physical rehabilitation will be needed as well. Surgery is not required for all ACL injuries.
For more information on problems of the knee and the treatments we provide, please call the office nearest you.
