 HIP FRACTURES
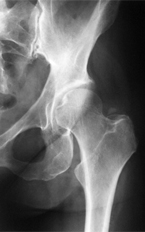
HIP FRACTURES
A hip fracture is a break in the top of the femur (thighbone) where the bone angles toward the hip joint. If the break occurs within two inches of the joint, it is called a femoral neck fracture. If it occurs between two and four inches from the joint, it is known as an intertrochanteric fracture. (A break further down the bone is classified as a broken femur rather than a broken hip.) Femoral neck fractures require more extensive surgery.
Hip fractures usually make it too painful for the person to stand. The leg may turn outward or shorten. They generally require hospitalization and surgical repair.
A person’s risk for suffering a hip fracture increases if he or she is over 65, female, or small-boned; has a family history of hip fractures; has osteoporosis or low calcium, which leads to bone weakness; smokes or uses alcohol excessively; is physically or mentally impaired; or takes medications that cause weakness or dizziness. Hip fractures are a common and serious problem for the elderly, for whom a simple fall in the home may be enough to break the bone.
HIP ARTHROSCOPY
Hip arthroscopy is a minimally invasive procedure used to diagnose and treat a wide range of conditions affecting the hip joint. This procedure can be used to confirm the diagnosis of various imaging procedures, such as X-rays and MRIs, as it provides your doctor with a three-dimensional, real time image of the affected area, allowing for the most accurate diagnostic results. If damage or abnormalities are detected during the diagnostic procedure, repairs can often be made during the very same procedure through minimally invasive techniques that provide patients with many advantages over traditional hip surgery.
During the hip arthroscopy procedure, your surgeon will make a small incision near the affected area of the hip and insert an arthroscope, a long flexible tube with a camera on the end that displays images of the inside of the hip joint on a video monitor for the surgeon to view in real time. During this diagnostic part of the procedure, your hip will be examined for any signs of tearing, damage or degeneration to the ligaments, cartilage and other internal structures.
If damage is detected, it can often be repaired through the same procedure by creating a few more small incisions through which tiny surgical instruments are inserted. These instruments allow the surgeon to replace damaged cartilage, join together torn ends, remove loose bodies or realign the joint to minimize pain and inflammation. Once the repair has been performed, the tools and arthroscope are removed and the incisions are sutured closed. A dressing will be applied to the area, which will later be replaced with smaller bandages while the incisions heal.
HIP REPLACEMENT
 Most damaged hips are the result of osteoarthritis or “wear-and-tear” arthritis, a degenerative type of arthritis that causes the cartilage to wear away over time so the bone ends rub together. Other common causes of hip degeneration include rheumatoid arthritis, trauma, osteonecrosis (bone decay), prior surgeries, and tumors.
Most damaged hips are the result of osteoarthritis or “wear-and-tear” arthritis, a degenerative type of arthritis that causes the cartilage to wear away over time so the bone ends rub together. Other common causes of hip degeneration include rheumatoid arthritis, trauma, osteonecrosis (bone decay), prior surgeries, and tumors.
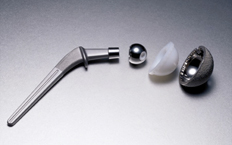
Joint replacement surgery removes the damaged, painful parts of the hip and replaces them with a prosthesis made of metal and plastic. The artificial joint can relieve pain and improve mobility when your natural hip can no longer do its job. An artificial ball and metal stem replaces the worn head of the thigh bone and a metal cup and artificial liner replaces the worn socket of the pelvis. The prosthesis allows the hip joint to move smoothly, so patients can enjoy a greater range of pain-free movement.
Total hip replacement is successful in over 95% of well-selected patients. On average, replacements last 15-20 years. Some patients enjoy full use of the prosthesis after 25 years or longer. Occasionally, an implanted prosthesis does not function as well as it was intended to. In this case, revision surgery may be performed to adjust or replace the mechanism.
For more information on problems of the hip and the treatments we provide, please call the office nearest you.
