Mathew Zin
"Matt is in his second year of Residency in the Family Medicine program at Stony Brook Southampton Hospital. When asked, Matt stated that he chose a career in medicine to further help people. “I saw my father (the first Dr. Zin) spring into action and use his skills during an in-flight medical emergency while returning from a family vacation. That moment was very inspirational to me, and I figured if I had the capability to do half of what he did, I could do some good in the world.”
Residents within the programs at SBSH are very much a second family to one another. “The best part about being a resident at SBSH is that there is always an opportunity to learn in a positive atmosphere surrounded by positive people. Everyone is willing to teach when asked and the other Residents feel more like friends rather than just coworkers.”
With a year and a half left of his training here, Matt is very much looking forward to the future. “I look towards the ability to continually refine my medical knowledge and apply the skills I learned here to propagate positive outcomes amongst my future patients.”
Mathew Zin
PGY-2 Family Medicine Resident
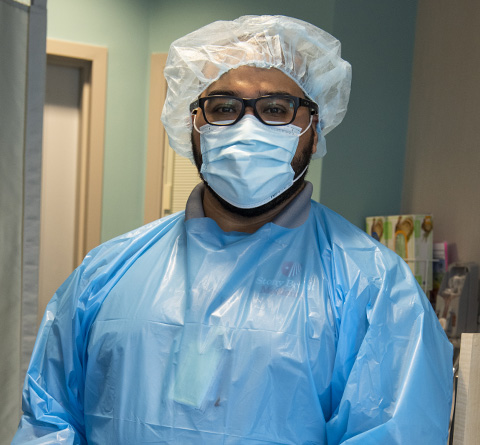
Matt Nier
Matt is under the bright lights of the OR and saving lives on the daily.
"General surgery residency is far more than cutting a patient open. We are taking care of medically complicated and critically ill patients, learning bedside procedures, understanding the complexities of anatomy during difficult operations, and working as a team to treat patients and make a difference in the community every day. One of the best parts of training has been getting to know my co-residents and working with truly remarkable attendings.”
Matt Nier
PGY-5 General Surgery Chief Resident
Massiel Battcher
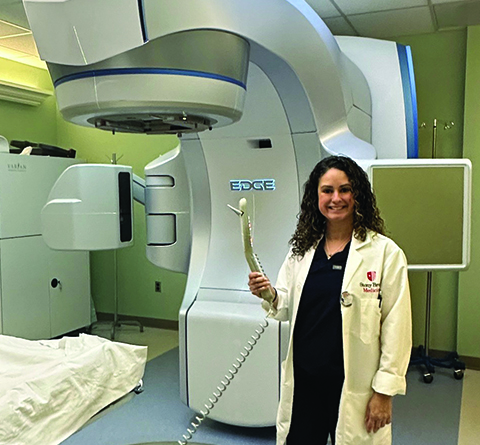
"My goal when I come into work every day is to make our patients feel comfortable and to get them through one of the most difficult times they will probably ever go through in their lives. I want every single patient to feel like they’ve made a friend when they come here. So, they don’t just come here for treatment. They come for a conversation and for human connection. I want it to be a pleasure for them as opposed to a medical appointment.
I treat patients who have been diagnosed with cancer with high-energy X rays to break down tumors with the hope to cure the patient of their cancer. We also treat patients who don’t necessarily have cancer - radiation can also be beneficial in tackling benign medical conditions. I've been doing this for a long time, and it’s an interesting story how I got into this field in the first place. My hairdresser was diagnosed with breast cancer. I was in college at the time, and I asked her questions about her treatments. She’d explained to me what she was going through. She knew I was in school and that I was interested in healthcare and science. She told me she could see me as one of those therapists that treated her. So, she really put this in my head. After some research, I eventually pursued it and realized this was exactly what I wanted to do. Luckily I was matriculated in the right place. It was science meets patient care, and that was perfect for me.
I actually received by undergraduate degree from Stony Brook University and then did a post graduate clinical program here and got certified. So, when I applied for a job here, it really became full circle for me. I’m working with my mentors, whom I have learned so much from. I really love the culture here. We make each other better every day so we can be the best that we can possibly be for our patients. I'm very appreciative for my colleagues because with them, our goal to provide individualized care is achieved daily. As busy as we are, we always prioritize the patient and make sure we are operating at 110 percent at all times. It’s the human aspect of it all that I connect with most. We are all human, and we need to be there for one another."
Massiel Battcher, BSHS, R.T.(T)
Radiation Therapist
Stony Brook University Hospital
Department of Radiation Oncology
Brendan Beecher
“I came to Stony Brook Eastern Long Island Hospital as a 3rd year medical student for my psychiatry clerkship,” says Brendan Beecher, DO, a 4th year Psychiatry Resident. “I thought I wanted a career in pediatrics, but I came here and found a passion for the work.”
Dr. Beecher hails from New York’s Catskill area and went to NYITCOM (New York Institute of technology college of Osteopathic medicine) before heading out east to SBELIH for his Psych Residency. He settled in Port Jefferson and says, “The North Fork is a place that feels the closest to upstate.”
“The work is very interesting and requires subtlety and patience,” says Dr. Beecher. “It allows me to connect with individual patients. Though it may challenge me, when it goes right, it’s really right. These are patients that people all care about here. I help people who may not get the help they need from other sectors and I’m happy to help.”
“I discovered in college that I wanted to go into medicine. It’s one thing to know about a specialty and another to get practical experience. Through my time here I discovered that it’s what I enjoy doing.” As Dr. Beecher concludes his 4-year residency journey, he realizes that “I want to focus on addiction medicine.”
During his residency, Dr. Beecher gained valuable experience at Stony Brook University Hospital and Stony Brook Southampton Hospital in addition to SBELIH. “The Psych program gave me a wide variety of experiences,” says Dr. Beecher. “Stony Brook University Hospital is very high-intensity. At SBELIH I got to hone my skills and explore my passions. The team at SBELIH has a local community feel. Here I’ve had the pleasure of working with attending physicians, nurses, and pharmacy staff with a collegial feel.”
Brendan Beecher, DO
Psychiatry Resident
Carrie Grattan
For the last 13 years, Peconic resident Carrie Grattan, RN, has focused on a career in nursing, “I worked as a bartender for years, but I found that nursing has the same pace and is also service-focused. With nursing, you help people in a very different way. I never thought I’d see myself in the profession, but I’ve grown to love it.” Carrie says that nursing, “came naturally to me.” “I was in oncology for 11 years before coming to SBELIH,” says Carrie. “There's a connection you make with a patient, and you feel like you’re part of their family. Nursing gives back as much as you give it. It’s never easy but you feel like what you’re doing has purpose.” Carrie was working as a nurse and in administration miles away from home before an opening came up at SBELIH. “I wanted to go back to basics and to find what I loved about nursing again. At SBELIH I was hired as a detox and med-surg nurse and it opened my eyes to the other side of nursing. It was much more emotional.” In April 2023 Carrie moved from a nurse on the floor to a management role, “I’m thankful for the amazing staff I have. They are thoughtful, hardworking, and they all work together to do what’s best for our patients. They make the ‘job’ part of the job easy.” “I love the community feel here,” says Carrie who looks forward to all the extra family time. “I’m so close to home and able to serve my community. Being part of patient care you understand that it is an honor to help your neighbors out. I’m so lucky to live 10 minutes from my job.”
Carrie Grattan, RN
Nurse Manager of 2N and ICU
Alison Caruana
"I work with patients who’ve suffered from an acute stroke. But the majority of what I do actually happens after a stroke occurs, meaning I work with patients and their families and help them to navigate obstacles, support in their recovery, and try to prevent another stroke from occurring. In the hospital, you often see patients at their worst. After they’re discharged, a lot of healthcare professionals might be left to wonder how their patients are doing after. Did that father get to walk his daughter down the aisle? Will this grandmother ever be able to speak or feed themselves again? In my role, I not only get to see the “after,” but I have the gift of being part of that journey. It often feels like you become part of their family. It’s beautiful. And then, on the flip side, sometimes recovery isn’t always so successful, so being there and seeing what you can do to make sure they have the resources they need means everything. It’s just very rewarding to be part of their lives like that.
A big part of recovery is healthy living, and I practice what I preach. I’ve actually been a runner for about 24 years. I currently run with a group of people early in the morning before work and on the weekends. It’s the best way to start the day. It helps me decompress, clears my head, and gives me perspective – all things that help me to be better in my work at Stony Brook. The physical and mental benefits of living a healthy and active lifestyle are endless. I’m also very competitive, so I love to race and participate in marathons.
As a stroke neurologist, time is of the essence in the short-term for recognizing and treating a stroke. That is less than a fraction of what a stroke really is. Stroke recovery is the marathon. There will be good days and bad days, just like parts of a marathon being great and other parts being challenging. Keep checking in with yourself. How am I doing as compared to last month? Two months? The year mark? And it’s important to not overdo it right after a stroke, either. Remember, it’s a marathon. Take it slow. Going too fast can counteract the healing of the brain that it needs to do naturally. It’s all about balance, and it takes time."
Alison Caruana, DO
Stroke Neurologist
Katelynd Collins
“When I was 13 years old, my mom – my best friend – was diagnosed with late stage breast cancer and given a 50 percent chance of living for five years. That was 25 years ago! She went for her radiation treatments right here at Stony Brook, which is when I was first introduced to the field. I’ll never forget coming with her one day, a scared teenager sitting in the waiting room, when a therapist here showed me the treatment machine. It was right then that I knew this was what I wanted to do. So, once I went to college, it all became about getting back to Stony Brook one day to work with the people who helped save my mom’s life.
As a radiation therapist, my job is to deliver accurate, safe and effective radiation treatments to our patients. But this is more than just a job to me, it’s personal. We are caring for a person’s life, for people who are loved and who have families. I truly believe the empathy I put into my work makes me better every day and allows me to provide my patients with the best care possible. There’s a big stigma around the word radiation. When people hear it, they often think of dangerous doses and atomic bombs...it’s scary. On top of that, people are often hearing that word while staring in the face of a terrifying diagnosis. So, all the radiation therapists at Stony Brook feel it's an important part of our job to put their minds at ease. We always try to calmly explain the procedure, make sure they are well informed and provide them with as much comfort as they need. It’s truly a pleasure to also get to know our patients on a more personal level, which not only helps to keep them in good spirits, but also makes us love our jobs more and more each day.
Lastly, when patients come in with their kids I always try and make it a point to show them around, just like I was all those years ago. Because it’s not just about caring for our patients, It’s also about caring for their families. You never know whose life you might change for the better.”
Katelynd Collins, R.T. (T)
Radiation Therapist
Stony Brook Cancer Center
Debbie Martocchia
“I love what I do,” says Debbie Martocchia, Phlebotomist/EKG Tech. “I started in beauty school and worked at a hair salon for a year. It wasn’t doing it for me at all. I had friends who were in the healthcare and suggested I check it out. I was interested in the medical field because there’s always action and you’re helping people.”
“My shift starts in the lab at 6 am where I pick up all the doctor’s orders for blood tests. I make my rounds and draw blood and do EKG tests,” says Debbie. “I start my day saying ‘hello’ and ‘good morning’ to all the patients and keep an eye on how they’re doing. Sometimes I notice things that I quickly report to the nurses to follow up. Communication is key.”
After a quick stop at the centrifuge, Debbie heads to Outpatient Testing where she and the team will see walk-in patients who stop in with doctors' orders for specific blood tests. “A lot of my patients have nicknames for me like Vampirella, Dracula, Sure Shot, Sharpshooter, and Needles. You make friends with patients you see all the time and develop a great rapport.”
“The lab techs are one big family,” says Debbie. “We do things together outside of the hospital from dinners to going to the beach and boating in the summer. It’s a nice relationship to have that closeness.”
In the hospital, Debbie says, “Phlebotomy plays a vital role in patient care. Phlebotomists are often the diagnostic detectives of healthcare. By drawing blood, we help the healthcare team figure out what is making the patient sick.”
Debbie is celebrating her 30th year here at Stony Brook Eastern Long Island Hospital as a phlebotomist but she jokes with a smile that she’s been here since the day she was born (because she was born here).
Debbie Martocchia
Phlebotomist / EKG Tech
Jessica Fenton
"Preventive medicine is the practice of trying to prevent people from getting sick. In other words, to give people practices to be as healthy as possible and set themselves up for a healthy lifestyle. Proper sleep, eating habits, stress management, exercise, social connectedness, and staying away from risky substances. And then there’s the business side of things: analytics, quality assurance and improvement projects.
I first got into family medicine and saw things that really frustrated me – homelessness and lack of access to healthcare and medicine. I couldn’t tackle these issues as a primary care physician. I wanted to help deal with these issues on a larger scale. I don’t think preventive medicine is something that’s very well advertised or well known. I just knew I wanted to help people to live their healthiest lives. When it came to looking for a residency in preventive medicine, I was looking for a program rooted in helping residents to find what they wanted to do and to reach their goals. I wanted a supportive community, and I found that at Stony Brook.
It's important to have a relationship with the people in the communities you serve. That’s the only way to provide the best care possible to them. You have to be involved in the community and find what they need and give them the resources to advocate for themselves. That’s exactly what I’m trying to do with a program called Styled Wellness. In April, we’re going to partner with barber shops and salons in the community and provide information on how to get insurance, spread awareness about heart health, provide different health screenings, and more. It's self-care meets health care.
I feel that residents push change and innovation, and that allows patients to experience innovative care. And that’s what I’m hoping to achieve with Styled Wellness – a different way of approaching public health issues and furthering our efforts in preventive medicine."
Jessica Fenton MD, MS
PGY-2, Preventive Medicine
Isabel Faringer-Perez
“I have a diverse background – my mom is from Sweden, and my dad is from Puerto Rico. I feel my background allows me to bring a different perspective to the work that I do as a midwife. I value culture, and birth is a very cultural event. People bring their own cultural knowledge and traditions that are oftentimes passed down through generations, and I try to value that and make sure my patients are seen and heard and that their culture is brought into their birthing experience.
I’ve always been fascinated by labor and birth from a young age. I remember always being very excited when my mother told us our birth stories. She came to the states as an adult and always knew she wanted a midwife to attend her birth as that is the norm in Sweden. I first became interested in the field of nursing when my father became very sick while I was in middle/high school. I saw what nurses did for him and how they advocated for him, and I wanted to be able to do that for others. I wanted to combine my love of pregnancy/birth/reproductive health with my passion for advocacy and caring. So, I worked towards nursing first, and a few years after began my midwifery education. I actually went to undergrad at Stony Brook University. So, to be able to be back here doing what I love means a lot.”
Isabel Faringer-Perez, CNM, MSN
Certified Nurse Midwife
Stony Brook Medicine
John Fazio
“I pass gas for a living,” said John Fazio, CRNA with a laugh when asked to explain what a Nurse Anesthetist does. “CRNA’s have a long history of giving the first anesthetics, around the turn of the 20th century. Now we’ve evolved into this advanced practice of nursing.”
“We learn to do things that other nurses aren’t trained to do,” John explained. “There are a lot of anesthetics that need to be given during a procedure or surgery in this country. CRNA’ s give over 50 million anesthetics per year and represent over 50% of the Anesthesia workforce. Here at SBELIH we use the ‘Anesthesia Care Team Model’ where an anesthesiologist and a CRNA work together. This frees up the anesthesiologist to do other things. And it’s safer for the patient to have two people focused on them providing excellent care.”
John started his healthcare career as a Pre-Med student at NYU before transferring to nursing, graduating in 1985. “I wanted to work in the ICU, with my first Nursing job being in surgical ICU (SICU) for three years. I moved into the OR briefly to work in the heart room. Then I applied to anesthesia programs after meeting CRNA’s who thought it would be a good fit for me.”
John and his wife Barbara, an OR secretary at SBELIH, migrated east to Greenport after the Chief Nurse Anesthetist called him about an opening. “The family closeness we have here means a lot to me. Leadership listens to what we have to say, and they are responsive to our needs.”
“In a community hospital we do a lot,” he says. “We work together with the Anesthesiologist to assess the patient, formulate an anesthesia plan, and stay with the patient throughout the peri-operative period. Vigilance is the most important thing about our profession.”
When he’s not in the hospital working with patients, John spends his time rocking out as the lead singer of the band POC alongside Dr. Lawrence Schiff, Vice Service Chief, Emergency Medicine SBELIH, and Dr. Ryan Zapata, also in the ER, and Andy Jepson. Rock out with John and POC on Friday, April 12, 2024, at Greenport Harbor Brewing Company in Peconic.
John Fazio, CRNA
Perianesthesia Nurses Week – Feb 4-10
John Reventlow
“Right out of high school, I found I was interested in pharmacy,” says pharmacist John Reventlow, RPh who grew up in Mastic Beach and now lives in Cutchogue with his family. “I’ve had my pharmacy license since I was 23 years old.” John has been an integral member of the Pharmacy team here at SBELIH for the past 21 years and a pharmacist for 30 years.
John explains that his dad helped him find his start, “My dad was a mechanic in Queens and fixed a pharmacist’s car. They were doing a job shadow where he worked and I was fascinated about how a tiny pill or an injected medicine could help someone.”
He got great advice all along the way, “I was accepted to St. John’s but instead enrolled in the pre-pharmacy program at Nassau Community College on the suggestion of an admissions counselor. It was a financially smart decision. In the end, I still graduated from St. John’s.”
“If you find something you love to do, and you’re passionate about it, it’s easy to come to work,” says John enthusiastically. “Working here we’re a very good team and everyone just jumps in. I don’t care how good of a pharmacist you are you need that support from pharmacy techs. The way Ray Krupski (Director of Pharmacy at SBELIH) has things set up here is very organized. I only had retail experience before coming here and Ray took a chance on me. In a hospital setting, it’s more about the medications and the health side as opposed to retail where it’s more about insurance and co-pays. Here I answer questions about blood pressure, reactions, and complicated inhalers when I work with the nurses.”
New drugs are developed each day and John says that what’s chosen for patients is driven by the doctors. “We discuss the advantages and disadvantages of the new drug in comparison to the existing drugs. Together we make the best choices for our patients.”
A typical day for a pharmacist starts at 7 am where the team goes over everything that occurred overnight. Then there’s a review of doctors’ orders and discussions with nurses to go over any questions about doses and follow-up medications. “I’m one piece of the big picture here. We interact with the nursing staff a lot to keep everyone in the loop and to stay on the same page for the good of the patient.”
John Reventlow, RPh
Pharmacist
James Kane
“When I was in elementary school, my uncle was diagnosed with cancer. So, I suppose healthcare was always in the back of my mind, but I never really put much thought into working in the medical field. I didn’t even know what oncology was. So, looking back, it’s crazy that I’m where I am now, working with patients who are fighting against this awful disease. And it’s amazing to see all of the strides that have been made in terms of research and patient care since when I was that little kid in elementary school.
At Stony Brook, I’m involved in the plan of care for patients at the Cancer Center. I oversee the scheduling of appointments and make sure patient visits go as smooth as possible. We serve as the connection between our clinical staff and patients. I really enjoy working in patient care and being a vital asset in our patients’ journeys. And it’s very meaningful for me to be able to do this right here in my community. Whether it’s a follow-up, infusion, lab work or an x-ray, I want our patients to know they can count on me.”
James Kane
Patient Disposition Coordinator
Stony Brook Cancer Center
Kristi Ladowski
"My job is to prevent injuries. Stony Brook University Hospital is home to Suffolk County’s only Level 1 Trauma Center for both adults and children, so I get to work across the entire age spectrum. The first step in preventing injuries is for us to really understand what’s happening in our community and how injuries are happening. We look at a lot of different data sources, such as the trauma registry, emergency department intake, police reports, mortality data, state-wide data and more. Then we use this information to identify the leading causes for injury and implement evidence-informed programs to address these mechanisms for injury in an effort to prevent them from happening in the first place. And for those injuries that do happen, I’m honored to be a part of a team of dedicated and skilled clinicians who can offer our patients the best chance for a full recovery.
Falls in older adults are the #1 injury that bring people to trauma centers. The good news is there are a lot of evidence-based programs that we implement free in the community that help to prevent falls. One of these programs is Tai Chi. Not only does this activity help to improve balance and prevent falls, but it’s also a mindful practice that helps reduce stress and encourages being in the moment. Stress is a risk factor for virtually everything so tai chi is really beneficial for your health overall. I’m actually a certified instructor, as well, and practicing tai chi has really improved my quality of life.
I love what I do at Stony Brook. I get to prevent bad things from happening and work with health professionals, a variety of health and human service organizations, and our community. I grew up on Long Island, so these are my hometowns and neighbors. I get to travel across the Island and meet people where they are. I get to be in their world and help enhance their quality of life. The connections I form with people are one of the most rewarding aspects of my job."
Kristi Ladowski, MPH
Injury Prevention and Outreach Manager
Stony Brook Trauma Center
Joseph Mulholland
"A big part of what we do out here is bridge the gap between people who need help with technology and anything with a power button that somebody many not be able to pick up right away. We try to make tech simple for people because it’s supposed to make our daily lives easier. We cover everything from printers and televisions to phones, networks and even the cash register in The Corner Shop. We do it all. We are small but mighty.
I love what I do, and I don’t think there’s many people who can really say that. I mean, I love it except for the waking up early part! It’s a community out here. I’m originally from the East End, and I’ve been working on the North Fork since 2013, so I recognize a lot of the people who come into the hospital. It’s comforting to see a familiar face and to know we are here for each other. And that’s also how I see my role at Stony Brook. I’m here to help people. Technology can be a struggle for some people, and I have the patience to work with them and help them to understand how to use devices and be more efficient. I like to think I’m helping to empower them and adapt to 2023. Also, in addition to teaching people new things, sometimes tech just breaks at inconvenient times and it takes a while to get it fixed. But I am here, and I always do my best to work as efficiently as possible. And I appreciate everyone’s patience along the way.
Tech was always a big part of my life. I’ve been a computer nerd and a gamer for as long as I can remember. And I like to figure out how things work. It started with Legos and evolved to the tech space, and here we are. I also always loved the beach growing up, and now I can walk outside work and I’m right on the water! Funny how things work."
Joseph Mulholland
Support Analyst
Information Technology
Stony Brook Eastern Long Island Hospital
William Powell
"I’m a life-long Long Islander, so to be able to work in my own community and do meaningful work is something I’m very proud of. I believe Stony Brook is the place to be. And I should know – I’ve been here for almost 23 years. In that time, I’ve been dealing with the business side of Stony Brook Orthopaedic Associates. We are the largest orthopaedic practice in Suffolk County and are continuously expanding our presence all over Long Island. I help manage the operations for the practice and am also heavily involved in financial planning, physician recruitment, human resources, facilities management, compliance and more. There is tremendous variety in my responsibilities, and that’s something I really enjoy about the work that I do. The other reason I enjoy what I do is that the orthopaedic surgeons here at Stony Brook are amongst the best. They are an incredibly talented and gifted group. And not only do they do amazing work, but they also teach and train the orthopaedic surgeons of tomorrow. I greatly respect our group of surgeons. The work they do really inspires and invigorates me.
Something else that’s really great to see working in orthopaedics is the positive patient outcomes. In this specialty, you often get to see immediate results, both surgical and non-surgical, and I speak from experience here. I’m a runner, and I often do 5K and 10K races. I’ve had every running injury that you can imagine, and I’ve been very fortunate to have had our physicians treat me. They literally keep me running. Our Department Chair, in particular, helped me through a recent running injury. I thought I was done, and now I’m back running and feeling great again. And that means I can help to keep Stony Brook Orthopaedics running and operating, as well!"
William Powell, MPA, CMPE
Administrator
Department of Orthopaedics
Stony Brook Medicine
Jennifer Reinhardt
“I grew up dancing. I performed from four years old all the way through my twenties. I always loved movement and the human body. When I was 16, I hurt my knee pretty badly and had to stop dancing for a while. My doctor put me in physical therapy, and that was when I first learned about PT. Over time, I learned that there were so many things you could do in the field, and that really interested me. Looking back, though, I’m not surprised I ended up in healthcare. Not only was my Mom a nurse, but I also volunteered at a hospital, and I loved it. Plus, I was always very good in science class, so that didn’t hurt!
That is a Level 1 Trauma Center. I did home care for a while, but I missed the hospital setting. I really enjoy the acuity and working with patients who are more critically ill. And the camaraderie and teamwork here are unmatched. We also collaborate with other teams quite often, such as Social Work and Care Management, and that’s something I really enjoy, as well – working together to help our patients as best as we can.
As physical therapists, we work as a team to make sure our patients stay mobile. We work with babies in the NICU all the way through to geriatrics. And for the past five years, I’ve been on the cardiothoracic service, working with patients who have had open heart and other vascular surgeries. It’s critical for patients who are very sick to get moving asap so they don’t lose the strength that they do have and to regain the strength that they once had. I find it so rewarding to be involved in the first steps of a patient’s recovery.”
Jennifer Reinhardt, MS, PT
Senior Physical Therapist
Physical and Occupational Therapy
Stony Brook University Hospital
Susan Wilner
I oversee operations for behavioral health at Stony Brook, Eastern LI, and Southampton Hospital, as well as our ambulatory sites. I help to operationalize new initiatives and maintain regulatory compliance, as well as come up with new ways to deliver services and improve access throughout the system. And when COVID hit, that meant telemedicine. It’s actually something I’d been working on for a while, but it went into warp speed with the pandemic. Telemedicine has always been important in order to help improve access to healthcare. COVID really highlighted the inequities in healthcare, but telemedicine is helping us to bridge some of those gaps. Part of our telemedicine efforts included giving tablets to our COVID units so providers could do virtual consults with patients who were positive for the Coronavirus. iPads were also given to patients so they could talk to their families outside of the hospital. We have also worked collaboratively between our hospitals to help bring services to where the patients are, but the services may not be. Most recently we began doing psychiatric evaluations on patients at Southampton Hospital from our providers at Stony Brook University Hospital in an effort to save the patients from having to take an ambulance trip from out East all the way to Stony Brook. This is helped us to provide even better care and a better patient experience to all of our patients, regardless of where they are located.
I still continue to do this work, but I now also spend a lot of time leading vaccine PODs here. This is the first time in a year that I’ve felt like I’m part of the solution. Up until this point, I’ve felt like I have been helping others to work, live and just simply function in a pandemic. But now, I feel like I’m helping us to get to the other side of this. It finally feels good.
Susan Wilner, LCSW
Assistant Director, Behavioral Health Services Operations
Jessica Marangio
Prior to COVID, I was an assistant director of nursing for adult inpatient Psychiatry. I did daily management of our adult inpatient Psychiatry unit and oversaw our nursing staff. Fast forward to the pandemic, where a lot of our patients were staying home and our unit census was as low as I’d ever seen. We needed to shift focus. We rounded in other units, which was very different for many. We were used to taking care of our own patients, and suddenly we were setting out to help our colleagues. As we continued rounds, we began to see a need and felt the pulse of the hospital - we saw a lot of sadness, exhaustion, and anxiety. We know the effects of trauma on a person’s mental health, and this was traumatic. We wanted to do more. We organized a fundraiser to make wellness baskets for every unit with calming activities, essential oils, teas, and snacks. We were then able to open an Employee Respite Area on 12 North, staffed 24-7 by our Psychiatric nurses who provided support, a calming environment, mindfulness activities, aromatherapy, meditation, a place to rest, snacks and beverages. We had over 19,000 visits to the area between April and July 2020.
I’ve since taken a position at Stony Brook Eastern Long Island Hospital to oversee inpatient and outpatient Behavioral Health services, but I can’t stress enough how important it still is to be careful. Wear a mask. Don’t gather in large groups. It’s just too soon. We really need to stay vigilant.
Jessica Marangio, MSN, RN, PMH-BC
VP Behavioral Health Services
Stony Brook Eastern Long Island Hospital
Amanda Waldeck
It’s been obstacle after obstacle but at the same time it’s been really empowering to see peoples’ resilience and how we’ve been able to adapt to all types of situations throughout the year. We’ve all adapted to this new norm of being overwhelmed. We are stretched so thin. We’ve all been pulled from our normal roles, which some days is harder than others, but we’re doing the best we can. Sometimes you’re juggling three roles at the same time, but it’s comforting to know that you’re helping and it’s for the greater good. I’m grateful to have the opportunity to do anything I can to help move forward and get past this together.
Amanda Waldeck
Clinical Pharmacist, Pediatrics
Barbara Mills
Everybody is tired. A lot of people thought we would have already cured COVID so we can all move on. But it’s not over. Our heroes - the essential workers who continue to sustain this momentum of work - are still working hard every day. Our rapid response team, in particular, is trained for this sort of thing. But even we needed to get creative. We are rescuing patients who get into trouble across all service lines throughout the hospital every day, as well as now caring for patients who have tested positive for COVID-19. In fact, our team is integral when it comes to intubating patients in COVID units. We even developed a plan when the pandemic first hit to work with respiratory therapists and anesthesiologists to safely intubate COVID-positive patients while limiting exposure to patients and staff.
I never thought I would see anything remotely related to a pandemic in my lifetime. But here we are. And the spread is more rapid now than ever before because people weren’t going anywhere during the quarantine. That’s not really the case anymore. But we are still here - taking care of our families and yours. We are not giving up. This has been traumatic for a lot of healthcare workers, especially those who had never worked, nor planned to work, in a critical care setting. But we’re doing what we need to do.
Barbara Mills, DNP, ACNPC, ANPC, PNP, CCRN, PCCN
Senior Nurse Practitioner
Clinical Assistant Professor School of Medicine
Director Rapid Response Team/Code Resuscitation
Director of Nurse Practitioners
Collette Castiglione
Our unit specializes in renal care, so we see patients before and after procedures; we prep them for surgeries; we take them for dialysis, endoscopies; and so on. Every now and then we have a rapid response situation, but that doesn’t happen very often. Well, it didn’t. But everything changed when the pandemic hit. I’d say the biggest change in our unit is how we approach patient care. We needed to limit exposure for ourselves and our patients, so instead of a bunch of people in and out of rooms multiple times throughout a given day, we would - and still do - cluster our care. I gear up from head to toe. I wear a gown, gloves, a mask, face shield, and a hair covering. Then, I enter a patient’s room and begin. Bathing, feeding, cleaning, taking vitals. Oftentimes, we spent two hours straight with one patient, which can be a lot when you have four, five, or more patients to care for. Even the vibe has changed on our floor. Patients used to be able to leave their rooms, walk around, and see their families. None of those things are happening right now.
When the pandemic first hit, everybody seemed to be in the hospital for COVID. It was Coronavirus all day, every day. Now, people are once again coming in for other medical reasons, as well, and some just happen to be COVID-positive. So in some ways, it’s even more complicated because care and treatments aren’t as streamlined. There is so much more going on, and to be honest, it’s exhausting. It’s so easy to burn out, and it’s not uncommon for people to put their mental health on the back burner. But it’s important to take care of ourselves in order to take care of others. What I will also say is that even though it’s still so scary, we know a lot more this time around. We now have knowledge and tools to tackle this second wave, and that makes me hopeful.
Collette Castiglione
16N, Med/Surg Telemetry Unit
Damaris Torres
One day, in the height of the first wave of the pandemic, I prayed to God in the hospital parking lot. I asked him to come to us and to help us. I then proceeded to walk into work and turned to my patients and colleagues and said, “Today, we are celebrating life! We need to be happy for today!”
My job is to help patients with whatever they need. Taking their vitals, drawing blood. But everything changed when COVID hit. Patient needs changed. And the way I connected with patients changed. We always do everything we can to brighten their days and provide them with love, hope, and the best medical care possible. But there is just something about this pandemic that opened our eyes and made us look differently at the way we provide care. And for me, personally, it made me realize just how important it is for everybody to remain in good spirits, especially when it’s really hard to do so.
I don’t think we should fear this virus. But we do need to respect it. We need to accept that this is our reality right now and adapt. We need to do what we can to protect ourselves and others.
Damaris Torres
Nursing Department
Grace LaTorre
As a Palliative Care physician, I care for patients with serious illnesses and those nearing end-of-life. The job of the Palliative Care Team is to support patients and their families and bring them together during a very difficult time. COVID has made this rather difficult, so we had to adapt and get creative. We’ve had to figure out a way to enable families to grieve and be with their loved ones. We have utilized technology like iPads and video chatting, which was challenging and didn’t feel natural at first, but we have adapted. And this wasn’t the only challenge we faced. We’ve had a tremendous increase in the number of patients we were supporting, and our consult volume across the hospital went up about 40 percent. We are working to our max, while at the same time sacrificing the time spent with our own families.
We’ve made a lot of headway in terms of how to deal with this pandemic, however, we are still in it. We are still seeing a rise in cases. I urge people to not underestimate or minimize the reality of what’s happening here. We are continuing to work as hard as we have been since the pandemic first hit. It’s real. It’s here. And we can address this together if we all continue to wear our masks, maintain social distance, and avoid large gatherings. Respect your life. Respect others’ lives. It is going to take all of us to really get through this.
Grace LaTorre
Director, Palliative Care Service, Stony Brook University Hospital
Program Director, Hospice & Palliative Medicine Fellowship
Director, Hospice & Palliative Medicine Education and Clerkships
Assistant Professor of Clinical Medicine
Ian Pak
COVID has changed everyone’s lives. It’s impacted our day-to-day. And it’s still very busy here. We’re seeing the post-holiday spikes, and it’s a good reminder to everyone that the virus is still out there, and we still need to maintain vigilance and follow the protocols that have served us well since March.
It’s been a really humbling experience to be part of the vaccine rollout to healthcare workers, specifically. These are the people who have been on the frontlines and saving peoples’ lives. The logistics of rolling out the vaccine to hopefully help protect everyone is an extra challenge, but I think we have the right group of people doing it, and we’re pushing forward.
Ian Pak
Pharmacist, administered the first vaccine at Stony Brook University Hospital
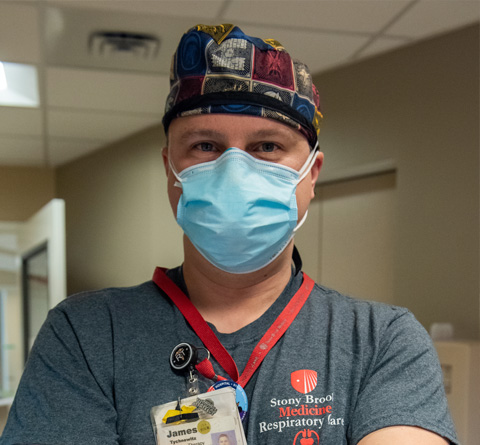
James Tychnowitz
Prior to COVID, I was working as a pulmonary educator, talking to patients about pulmonary diseases and how to manage themselves. I don’t think people knew what a respiratory therapist was before the pandemic. It’s not a role you’d normally see in shows like Grey’s Anatomy, and it’s not something you would really even think about unless you or someone you know needed to be put on a ventilator. But then COVID hit, and everything changed. I became exclusively focused on managing pulmonary medications and taking care of ventilators – life support machines. When this all started, we were navigating uncharted territory, forced to treat an unknown and figure out the best management strategies to keep patients alive.
Everything was so chaotic. Whenever a patient comes off a ventilator, we play chimes. But I’d be lying if I said I remember the first time I heard the chimes. Time feels compressed when you are exhausted because of the daily rigorous care you are providing to the most affected patients of the pandemic. The virus is a vulture waiting to latch onto people who are most at risk. However, I am hopeful. There is a light at the end of the tunnel, and that speaks to the hard work everybody is doing to make that possible.
James Tychnowitz
Respiratory Therapist
Jennifer Leone
Every day when I leave the hospital and drive home, I look up at the bright blue sky, and I cry thinking about what I just left behind. I hate leaving work because help is always needed. My job is to transport patients throughout the hospital. This didn’t change when COVID hit, but my life certainly did. The number of patients we move on a given day has grown tremendously, and we now need to put on proper PPE before we can even be with a patient. But the biggest change of all is not being able to interact with patients the way we used to. Moving with patients from point a to point b allowed us to talk to them. This is our way of getting to know them and providing comfort. But patients with COVID have a hard time breathing and are often hooked up to oxygen, so they can’t really talk. That doesn’t stop us from doing what we do, but it’s different. I still talk to patients and have them nod or give a thumbs up. I will always do anything I can to provide comfort. I even visit patients during my breaks on occasion because it can be lonely for them, and sometimes you just need somebody to talk to.
The pandemic has really made clear we are all a team at the hospital. We in transport help the nurses as much as we can - especially right now. But it’s not easy. I am exhausted. According to my watch, I walk about eight miles per day within hospital walls. But I have to say, I have never been more proud to have a job than this one at Stony Brook.
Jennifer Leone
Transport Distribution
Joshua Miller
I received a call from Dr. McGovern in early March outlining the need for a community-facing on-site COVID-19 testing location at Stony Brook University’s South P-lot, and I was asked to help oversee clinical operations. Prior to the pandemic, my job as medical director of our Clinically Integrated Network was (and still is) to ensure that patients receive the highest quality of care anywhere they go within the health system. I also oversee Stony Brook Medicine’s diabetes program. But when I got that call about the testing site, every appointment on my calendar needed to be pushed to focus on this high-priority initiative. And the testing site wasn’t the only priority. We quickly realized the profound impact that COVID-19 has on hospitalized patients with diabetes. I found myself at the testing location in the mornings and at the hospital in the afternoons, rounding with our diabetes team on critically-ill COVID-19 patients with diabetes in the ICU. And then meetings, of course, were done at night.
While things seemed to be looking up for a while over the summer months, we are now in the midst of a second and more challenging wave. Many are exhausted. But healthcare workers cannot give in to COVID fatigue; we must persevere. We are continuing to fight this virus to help our patients and our team get through these challenging months ahead. All we ask is for people in the community to continue to be diligent about safety measures and help to prevent the spread. I am inspired by my colleagues in healthcare who have given tirelessly to help patients and support one another through these unprecedented challenges and remain #StonyBrookStrong.
Joshua Miller
Assistant Dean for Clinical Integration
Medical Director of Diabetes Care
Manny Taveras
I am part of a vital operation at Stony Brook. My job is to deliver linens throughout the hospital every day, regardless of the circumstances. Whether it’s a towel, blanket, or gown, you need to have clean linens in a hospital setting. We even provide hypoallergenic linens for those who need them. Nothing but the best for our patients. It all comes back to providing comfort and the best possible care. And that continues to be the case, even throughout the pandemic. A lot changed, though, behind the scenes when COVID hit. More patients means we are a lot busier. And we take so many precautions now to keep ourselves and others safe. The first few months of the pandemic were particularly scary for me. I worried about bringing something home to my family. We slept apart because I was afraid I might infect them. It was mentally exhausting - and still is, sometimes.
Everybody who works in this hospital is working extremely hard. We are battling every day. I’m proud to work at Stony Brook, and I’m proud to be in my department. We are all pushing forward together.
Manny Taveras
Linen Department
Michael DeMasi
My life has changed dramatically since COVID first hit. Obviously social distancing, isolation, spending holidays exclusively with my nuclear family, things like that. But in terms of what I do here at the Hospital, I am largely involved with obtaining the PPE and supplies that are critical for taking care of our patients and keeping our staff safe.
I never expected to be working in the midst of a pandemic. It’s a tremendous challenge because the demand for supplies and resources is throughout the country now – not just Long Island and the New York area. But I do see a light at the end of the tunnel. We’re not there yet. We still have a long way to go. We’re in the midst of a second wave, but we can get there. We just have to stay the course. And to anybody who thinks this is no longer a problem, I would say: I wish I could walk you through some of the floors in the hospital, and you can tell me it’s not a problem.
Michael DeMasi, RN, MS
Director of Clinical Value Analysis, Stony Brook University Hospital
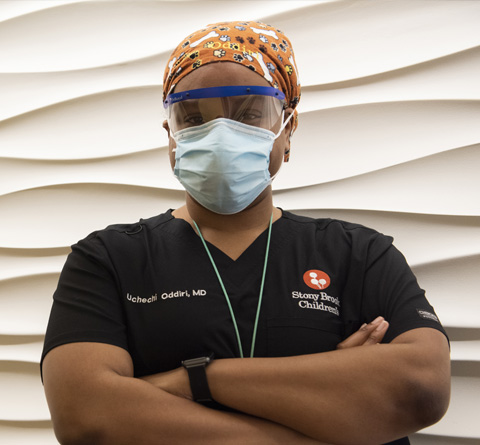
Uchechi Oddiri
I typically care for critically-ill patients from infants to adolescent children. We have a huge breadth of acuity in our unit. But when the pandemic hit, we were faced with doing something we typically didn’t do in our day-to-day. We pitched in to help care for adult patients. This actually turned out to be a very eye-opening experience. We had adult patients introduce us to their kids on FaceTime, and many of us being parents ourselves, it just hit us. It could just as easily be any one of us in that hospital bed. You don’t feel that as much when caring for patients so much younger than you. It really helped us to empathize on a whole new level. We also had a spike in our younger patients coming in with post-COVID Multisystem Inflammatory Syndrome in Children, which was something else we had never seen before. It was just all uncharted territory, but we stepped up. We showed strength and resilience because we had to – for our patients. I think it’s helped us to become better doctors and better people. We were tested, and we proved to ourselves that we can reach higher limits than we ever thought possible.
Uchechi Oddiri, MD, FAAP
Clinical Assistant Professor of Pediatrics
Stony Brook University Renaissance School of Medicine
Pediatric Intensivist, Stony Brook Children's Hospital
Mike Cullen
I’ll never forget my first experience with COVID-19. I went up to the CEO’s office, and Senior leadership was all there. They told me they needed us to renovate a floor ASAP. So, that’s exactly what we did. In just three days, we completely updated and transformed a floor to accommodate COVID-positive patients. I was so impressed with and proud of my team, and that pride only continued to grow as things escalated. We also secured and installed 95 negative pressure machines to filter the air in COVID-positive patient rooms, which was no small feat. It was just teamwork I had never seen before. Plant operation, housekeeping, project management, construction, architecture, nursing – everybody worked together amid this uncharted territory. And I had a whole new level of appreciation for every single team and department at Stony Brook. Everybody understood the risks and did what they needed to do. And they still are.
The pandemic just feels so surreal. It’s something you can’t make up. Even just being on a COVID floor in the hospital – it changes your life. I guess at the end of the day, all I have to say is a lot of special people work at Stony Brook.
Mike Cullen
Associate Director of Facilities and Support Services
Molly Rago
I work at the Stony Brook Cancer Center and help get patients onto clinical trials for different treatments, radiation, surgery, and other interventions. I help get them into the studies and monitor them throughout their time in the trials, as well as during follow up. When COVID hit last spring, I was reassigned to a COVID-19 study that was meant to take donated plasma from those who recovered from the Coronavirus and infuse it in existing COVID-positive patients. The study has since ended, but I am definitely keeping busy back at the Cancer Center. COVID changed a lot for cancer patients. Not only do they have an extra layer of concern being immunocompromised, but they can’t have loved ones physically with them right now while they receive treatment. It’s an extremely difficult time for everybody.
While being called a hero is flattering, I don’t really consider myself to be one. Or at least I’m no different from my colleagues. Everybody has been impacted by COVID, and everybody has stepped up. In my book, everybody is a hero.
Molly Rago
Oncology Research Nurse
Harold Rivas
COVID is a public enemy – but one we can’t physically see. It’s something that required us to step up and do things we’ve never done before. What that meant for my team was surface and airborne decontamination using a hydrogen peroxide vapor technology. Everything that involved patients and healthcare professionals was cleaned with this new technology. Patient rooms, nursing equipment, cell phones – you name it, we cleaned it. And I have to say, I don’t consider myself a hero. My staff are the heroes in all of this. They are the ones facing the pandemic every day, and I am just here to support THEM.
I honestly never thought I would experience something like this. But it’s taught me a lot. For example, don’t be selfish. Nobody is immune to this, and you never know when the virus is going to touch your life, if it hasn’t already. This is no joke. We need to stay alert. And if you have the opportunity, get vaccinated.
Harold Rivas
Supervisor, Housekeeping
Wilfred Farquharson
Historically, systems are set up that oppress and discriminate and make typical daily functions more difficult for those in the LGBTQ+ community. Psychiatry and psychology also have a long history of mislabeling sexual and gender identity as “disorders,” further marginalizing and oppressing this community. This is why proper mental health and emotional support are key components in LGBTQ+ healthcare and overall well-being. I think a lot about this in my profession, particularly in the context of those who are doubly or triply marginalized. There are voices that don’t get heard as much as they should. Some never at all. That is why participating in the LGBTQ+ Health Needs Assessment Survey is important. What is it like for somebody who is part of both the black community and the LGBTQ+ community? Well, the survey will allow these stories to be told. We will be able to more clearly see and better understand this intersectionality as well. The complex marginalization of being Black and a member of the LGBTQ+ community has led to people being overlooked far too often as this group seeks the acceptance and validation they deserve. I also try to give people a platform in my own way, I run a transgender adolescent group, where we talk about gender and what young people are dealing when it comes to misgendering, dealing with discrimination in classrooms and hallways, and more. And I do this work as a heterosexual black male. I understand marginalization and power imbalance, and I use this to inform my allyship.
Wilfred Farquharson IV, Ph.D. (He/Him)
Clinical Assistant Professor of Psychiatry and Behavioral Health
Licensed Psychologist
Director of Child and Adolescent Psychiatry Outpatient Clinic
Polly Kanganis
“Healthcare is important for everybody, but unfortunately, some patient populations are marginalized. I want every patient to know that they are welcome in our office. We want you to feel safe and validated, and we want you to know that your privacy and choices are respected. That’s what I’m all about – the patient experience. More specifically, I am a board-certified ob/gyn and an attending gynecologist at Stony Brook. I do exams, work with patients who have STDs and STIs, etc. I also see a lot of patients who are taking hormones, whether that’s contraceptives or hormone replacement therapy for patients going through menopause or those who are transitioning. The patient journey is unique to every single person, and that should be respected and celebrated.
Participation in the LGBTQ+ Health Needs Assessment Survey is important for members of the LGBTQ+ community on Long Island. It will allow us to identify gaps in the healthcare system and help us to figure out how to fill said gaps. No patient should hesitate when it comes to seeking out healthcare services for fear of lack of respect in communication or privacy. So, awareness and participation in this survey is critical. Everybody deserves the best care possible.”
Polly Kanganis, MD, FACOG (She/Her)
Obstetrics & Gynecology
Smithtown Women’s Health, Stony Brook Medicine
Website: https://www.stonybrookmedicine.edu/smithtownwomenshealth
Phone: (631) 265-4567
Ted Uotani
“As a member of the LGBTQ+ community, I believe healthcare focused on LGBTQ+ needs is crucial. I had a recent experience that I faced where I had to be an advocate for myself and my healthcare needs at the doctor’s office. This doctor was unfamiliar with certain LGBTQ+ focused healthcare needs. As a healthcare provider, myself, I understand how valuable an open and honest conversation between provider and patient can be in establishing trust, as well as working together to make the best decisions for the patient. I have been fortunate to have had previous providers who have opened this discussion with me and provided me with valuable information, as well as resources, so that I could become aware and better educated. Together, my doctor and I could make the decisions that could promote my health in a comfortable, safe manner. This is why I believe participating in the LGBTQ+ Health Needs Assessment Survey is important. We need to bring awareness to our healthcare providers so that they can become informed and educated about LGBTQ+ healthcare needs. As healthcare providers, we undertake this responsibility to do what’s best and right for our patients. Although my profession is not specific to LGBTQ+ healthcare, the basic principles of communication and respect still hold true. My patients have special needs, and I feel that it’s my responsibility as their provider to be able to have these open, sometimes difficult, conversations with all assigned to their care so that we can give each patient the best care for them. Advocacy can take place in many different places and different forms, but even the smallest step can help bring awareness to providers of communities that may be underserved.”
Dr. Ted Uotani (He/Him)
Clinical Assistant Professor of Psychiatry and Behavioral Health
Special Needs Dental Fellow
Stony Brook Medicine
Connie Kraft
"Our role is to keep the hospital prepared and ready to respond to emergencies. Whether that means inclement weather, mass casualties, or even a pandemic, we take care of planning, training, reviewing and evaluating plans, and overall just being ready for when those things happen. I’ve been working on pandemic planning for many years now. It’s been on hospitals’ radars for quite some time. Resources, patient surges, infection control – we planned for it all. I am unbelievably proud of our staff for what they have done throughout the COVID-19 pandemic. It was uncharted territory for many, and everybody just stepped up and did what needed to be done.
Our EMS agencies are first responders. They are heroes. They are oftentimes the difference between life and death. They are on the scene when people are in trouble, whether it’s a health emergency or a traumatic injury. They are highly trained and able to respond very quickly and effectively, and they get patients to the right place with the right care. Many times that’s Stony Brook University Hospital’s Level I Trauma Center. That’s actually where I first became familiar with Stony Brook’s EMS agencies. I used to be a transport nurse in the Emergency Department, and I worked side-by-side with our EMS transport office, both ground and air. These people are truly amazing. They are disciplined, they work as a team, and they have a level of expertise that is simply unmatched."
Connie Kraft, RN, MSN, MS, CEN, CNE
Emergency Manager
Department of Emergency Management
Stony Brook Medicine
Justin Waryold
"One of my focuses over the past 13 years has been to provide culturally-competent care to the LGBTQ+ community. Historically, this population has never really been able to truly access culturally-competent healthcare. They have always had barriers. I, however, am a provider who supports this community. I see myself as a partner in my patients’ healthcare. The fact of the matter is that we simply need more providers who listen to their patients and understand their concerns; providers who don’t judge their patients for who they are, how they express themselves, or how they identify. I think there are a lot of providers out there who want to help their patients in this community but just don’t have the knowledge and tools to do so. That’s why participating in the LGBTQ+ Health Needs Assessment Survey is important. It has the potential to give providers on Long Island an opportunity to better understand the healthcare needs of patients in the LGBTQ+ community.
I understand what patients in this community are looking for, and I am always open to continuing to learn and grow. Simply put, I listen to my patients. I don’t just assume. I set the tone for a safe and comfortable environment. I ask what their preferred names and pronouns are. I provide services such as PEP, PrEP, STI testing and gender affirming care. I meet my patients where they are and provide the best care possible so they may live long and happy lives."
Justin Waryold, DNP, NP-C, GS-C, FAANP (He/Him)
Nurse Practitioner
Partners in Primary Care
Website: https://www.partnersprimarycare.com
Phone: (631) 418-8069
Caitlin Feeks
“The care of children is extremely specialized. Children are not simply little adults. The ways they present illness can be very subtle and often overlooked by someone who doesn’t have a trained eye. Here at Stony Brook Children’s Hospital, we are able to provide that specialized care. And we provide a calmer environment for our patients, as well. Kids don’t need to be in the midst of adult illness, which can sometimes be scary for them to see. The minute a child walks into our facility, I think they feel like it’s a safe place. It evokes a playful, trip-to-the-aquarium type of feeling. And it can settle a parent’s anxiety, as well.
I love working with kids, so going into pediatrics was an easy decision for me in medical school. And as I became more familiar with the world of pediatric emergency medicine, it became clear that’s where I wanted to be. I enjoy the fast-paced environment and being able to see immediate results from the work that I do. I feel anything but stagnant in this area of medicine. And it’s not just what I do, but it’s also where I’m doing it. The people in our pediatric ED are a team. I was an athlete growing up and always loved that team environment. And that’s what we have here at Stony Brook. Everybody steps up and puts their best foot forward so we can provide the best care possible.”
Caitlin Feeks, DO FAAP
Clinical Assistant Professor, Department of Pediatrics
Attending Physician, Stony Brook Children's
Joseph Giglio
"I played a lot of sports when I was younger: football, hockey, baseball, to name a few. I ended up injuring my knee and had to have surgery. And that’s when I knew...physical therapy was the profession for me. As physical therapists, it’s our job to help patients make a safe transition into their next level of care and help them to maintain an optimal, functional life. And we treat patients with all kinds of ailments. Whether it’s a physical injury or a medical/surgical condition, physical therapy often plays a role in the recovery process. It’s ageless, as well. It doesn’t matter if you are a neonate or centenarian; physical therapy can help if you need it.
I’ve been at Stony Brook for 29 years now, and I have to say, it’s a wonderful place to be. It’s a tremendous learning environment, and I am afforded the opportunity to work with the greatest people every day. The teamwork is foundational here, and it’s something we should all be proud of. A perfect example of that teamwork is this past year. In all my years here, I have never experienced anything quite like the pandemic. We were all scared because we didn’t know a lot about COVID. But we pushed that fear aside and did what we needed to do. We all worked to mitigate the spread and protect our patients, staff, and community. And I am so proud of my staff for stepping up the way they did. We even conducted a special program, in partnership with Rec Therapy, called, “Breathe, De-Stress, Exercise.” We went to COVID units throughout the hospital and tried to help staff get through this time with yoga, stretching, and by being there if they needed someone to talk to. Despite all of this, I don’t consider myself a Healthcare Hero. I took an oath to practice physical therapy and treat patients who are sick. It’s my responsibility, and I don’t take that lightly."
Joseph Giglio, MA, MS, DPT, CWS
Interim Supervisor of EEG
Associate Director of Inpatient Physical Therapy
Sherif R.Z. Abdel-Misih
"I wear several hats at Stony Brook, all of which help to make me both personally and professionally fulfilled here. My clinical focus is surgical, mostly concerning gastrointestinal and abdominal cancers. I also do surgical education, currently acting as program director for surgical resident training. As a surgeon, you can only help one patient at a time, but as an educator, you have the ability to impact countless patients through training our future surgeons. And lastly, I also sit on a number of committees that look at the big picture, reviewing institutional practices and such. To summarize, I try to leverage my interests and strengths here in hopes that I can make an impact in this community.
I embrace some of the most advanced cancer cases to not only challenge myself, but more importantly, to provide these patients with the best care possible. And that care is not limited to the technical aspects of surgery. In medicine, we have come to understand there are things that happen to patients related to a disease that are physiological, of course, but then there’s also the psychological impact, the recovery, and getting them through the many challenges they may face. I enjoy the interactions and relationships I develop with my patients. I believe it’s important to help them to manage the psychosocial factors of a disease, as well as the disease, itself. In other words, I like to figure it out and fight with them. And I do all of this in collaboration with an incredible, multidisciplinary team. Together, we remain innovative and dynamic in the ways in which we approach the diseases we face."
Sherif R.Z. Abdel-Misih, MD FACS
Associate Professor of Surgery
General Surgery Residency Program Director
Stony Brook Medicine Department of Surgery (Surgical Oncology)
Stony Brook University Hospital
Joan Nastasi
"I was called to the profession of midwifery as it allows me to support and care for women. As a midwife, one of my responsibilities is caring for postpartum parents who choose to breastfeed, and Stony Brook University Hospital affords me the opportunity to provide evidence-based midwifery and lactation services to diverse populations.
As an International Board Certified Lactation Consultant (IBCLC), I am a strong advocate for breastfeeding (when one is able to, of course). While it is normal for new parents to experience fear of the unknown surrounding breastfeeding, the Stony Brook Midwives are here to support new parents and babies with lactation services. With proper guidance and support, most women are able to successfully nurse. The benefits of breastfeeding for both parents and babies are endless. Optimal nutrition and reducing the risk of diseases and depression are just the tip of the iceberg.
Here at Stony Brook, lactation support is open to all patients and not just those who are cared for in the midwifery practice. Our appointments can serve a variety of needs ranging from the fundamentals of lactation and providing skilled support for parents in their breastfeeding journey to assisting parents in developing a pumping plan for their return to work. As part of providing lactation support to the Stony Brook community, I personally had the privilege of preparing and guiding my daughter and family through a successful, exclusively breast fed grandson who was born at Stony Brook this summer."
Joan Nastasi, CNM, IBCLC
Midwifery/Obstetrics & Gynecology
Harry Mushlin
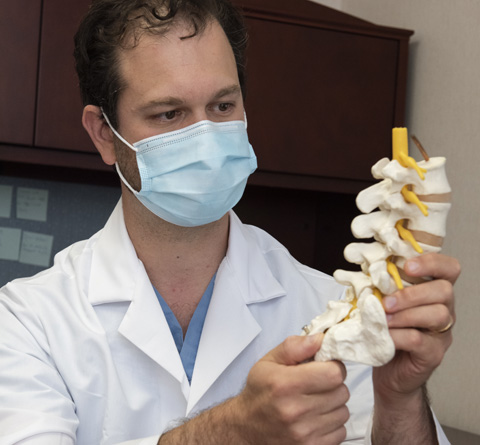
"I studied cognitive neuroscience in college. The subject matter was the right fit but it wasn’t hands-on enough for me. It wasn’t until I eventually discovered surgery, and more specifically, neurosurgery, that I found a field I was willing to dedicate my life to. Within neurosurgery, it’s spinal disease that really interests me the most. It’s extremely varied in terms of the cause and types of surgeries, and I thoroughly enjoy helping people with these problems.
Fast forward to now - I’m fellowship-trained in complex and minimally-invasive spine surgery. From trauma to degenerative disease and scoliosis - what I deal with runs the gamut. The specialized extra training I received in spine gave me a unique toolbox of surgical skills necessary to offer each patient the highest standard of care available. This includes minimally-invasive techniques that can lessen blood loss and recovery time, to help people get back to their everyday activities faster. I also have additional training in neurotrauma. Helping patients and their families get through devastating and unexpected injuries is something I’m passionately committed to.
One of the most important things I’ve learned is that being a strong doctor or surgeon is more than just being surgically skilled. It’s also about creating a balanced approach — an agreed-upon therapeutic plan that’s aligned with the goals and expectations of both the patient and doctor. This is a critical part of my practice. I listen to my patients closely. I understand how the body functions and bring the latest techniques and approaches to the table to help patients meet their goals. I’ve dedicated my life to this work, and I’m glad to be doing it at Stony Brook now. I am very excited to be serving this community."
Harry Mushlin, MD
Neurosurgeon
Neurosurgical Director, Complex Spine and Deformity Program
Caitlin Gibney
"My job is to help coordinate the day-to-day functions and meetings for our Chief Nursing Officer and Vice President for Patient Care Services at Stony Brook Southampton Hospital. I also assist all of our nurse managers and nursing supervisors with any needs that will enhance their ability to do their best work. My work has been particularly rewarding throughout the pandemic. It’s been so challenging on the staff, so whatever I can do to put a smile on someone’s face, make their lives easier, or recognize the sacrifices they make every day is just really important to me. I always wish I could do more, but I do feel satisfied knowing I am doing what I can to help, regardless of how big or small a given task might be.
Stony Brook Southampton Hospital is a special place. The level of care and compassion given to patients is unmatched. And internally, we just have the best people working here. Everybody is so supportive. I always try to make people feel as supported and welcome as when I first started here. I have an open door policy, and I always want people to know I am here for them. We are like a family. I look forward to my future here as I continue to grow with Stony Brook. In fact, I see myself here for quite some time."
Caitlin Gibney
Administrative Assistant to Chief Nursing Officer & VP, Patient Care Services
Stony Brook Southampton Hospital
Anne Walsh-Feeks
"I love what I do at Stony Brook Medicine - overseeing our ambulatory practices and making sure people have a quality, uniform Stony Brook experience. But my job drastically changed when COVID hit, and more specifically, when we started hosting large vaccination events. We had never done this before, but led by Dr. McGovern, we got together as a team and figured out how to do mass vaccinations safely. We chose to do a number of events in Commack, so we put a plan together for how to get people through the door quickly, provide them with medical consultation should they need it, get them vaccinated, have them observed, and help them to schedule their second dose. This experience gave me a chance to work with hundreds of Stony Brook employees I’d never even met before. We all had our day jobs, and then we’d go there on the weekends for back-to-back vaccination events. You’d think people would be exhausted, but the energy level was amazing. You could see the team smiling underneath their masks. The enthusiasm never waned. It was also a very emotional experience. People were so happy to be vaccinated. Once, a florist came in and gave a tulip to every single person working the pod. I will never forget that day. My job has morphed into something bigger than myself over the past year and a half, and I could not be prouder to be doing this work and to be leading the team that I do.
I’ve worked for other healthcare systems before, but when I had the opportunity to come to Stony Brook, I came because of the leadership and the culture here. And it’s actually something my daughter sensed, as well. She’s in pediatric emergency medicine at Stony Brook. We never would have thought our paths would cross professionally like this. But we both felt the people, the culture, and the mission here were just right. It’s that team-oriented structure and spirit that, amongst other things, sets Stony Brook apart."
Anne Walsh-Feeks, MS, FACHE
Assistant Dean and Chief Operating Officer
Ambulatory Operations
Jennifer Hacker-Johnson
"Art is its own language. Sometimes we don’t have words to express the experiences we go through, and art can fill that gap, acting as our vehicle of communication. Art and written expression are, admittedly, an unusual approach in a hospital setting. But I’ve been doing it for 16 years, and it works. We make people feel seen and heard. Our sessions are strategically developed with our patients in mind. What are they struggling with? What do they need? Whether it’s a group activity or a one-on-one session, we’re always exploring feelings and enhancing perspective.
Hospitals are a difficult place to be. But it’s clear to me that our patients benefit from art therapy. Of course we need science but the addition of art can very effectively inform medical treatment. It’s also where we are able to get a better understanding of whom the patient is. Their illnesses and struggles. We had a patient once who had some real behavioral struggles. They were really aggressive and volatile. It was very clear they struggled with emotional regulation. But you saw their best self when we did art with them. The improvement over time was magnificent. And they even continued art beyond their stay at the hospital.
Simply put, art is an important service to have."
Jennifer Hacker-Johnson ATR-BC, L-CAT
Art Therapist
Tara L Kaufmann
"I was first introduced to #dermatology during a summer clinical research project while I was a medical student at Stony Brook University. I quickly realized the field of dermatology was broad and exciting, and it really resonated with me. Dermatologists treat both acute and chronic patients, perform many procedures including skin cancer surgeries, and contribute to the development of medical therapies through clinical research.
One of the most important things we do as dermatologists is diagnose and treat skin cancer. It’s important for people to be aware that even a small new or changing mark on their skin could potentially be a serious medical issue. It is supremely gratifying to enter an exam room and use my trained eyes and clinical acumen to diagnose a patient’s condition and moreover, to see their impassioned relief that we have not only identified the condition, but also, and more importantly, we have a treatment plan.
Stony Brook Dermatology provides cutting-edge treatment with a personal touch. Not only are we interested in our patients’ medical conditions, but we also want to understand their lives.
We strive to provide wonderful care allowing science to guide our treatments, but never forgetting that the patient is a person, and that they always come first."
Tara L Kaufmann, MD, FAAD
Clinical Assistant Professor, Vice Chair
Department of Dermatology
Adrienne M. Haughton
"My goal is to have a transformational impact on people, and dermatology allows me to do that. If you can help someone improve their dermatologic condition, it can have a significant impact on them psychosocially. For example, skin and hair are easily seen and can cause people a lot of anguish if it’s something they are struggling with. And if we’re talking about a life-threatening disease like skin cancer, you can even save, prolong or enhance someone’s life.
I came to Stony Brook because I wanted to spend some time teaching residents, in a collegial environment, and treat patients holistically using a multidisciplinary approach. I have to say I’m quite pleased. The physicians here are at the forefront of therapeutic, medical and surgical treatment options and are invested in providing the gold standard of care to patients. I’m proud to be part of that. Being at Stony Brook also allows me to really focus on treating patients with alopecia, which is a great example of how dermatological issues can impact people regardless of age, sex or race. I’m a local expert in the treatment of hair loss, and I understand just how anxiety-provoking it can be. Therefore, if you are struggling with this and you decide to come and see me, you will receive a thorough evaluation and diagnostic approach and comprehensive treatment regimen."
Adrienne M. Haughton, MD, FAAD
Clinical Assistant Professor, Director of Medical and Cosmetic Services - Commack
Department of Dermatology
Stony Brook University
Christine Russo
"I was with my husband and six-month-old son at JFK Airport in early December. We were waiting to go through security when my husband urgently tapped me on the shoulder. I turned around to see a young woman seizing on the ground. I immediately lifted my son out of my carrier vest, handed him to my husband, and ran over to the woman. At this point, the woman was not breathing and lost her pulse. I started chest compressions and instructed someone to get me an AED. We administered three shocks to this woman and continued chest compressions for about 20 minutes. EMS finally arrived and confirmed that the woman had regained a normal cardiac rhythm after our interventions.
This was my first time administering CPR outside of a hospital setting, which has less than an 8 percent survival rate. This was a perfect example of how early defibrillation and high-quality CPR can make the difference. They can literally save a life. A colleague said to me that not a lot of people would do what I did, but I disagree. I think that more people would absolutely help if they knew how. Less than a third of cardiac arrest victims get bystander CPR, and education can help close that gap. My CPR certifications made me confident in the care I delivered in this woman's time of need."
Christine Russo, MSN, CPNP-PC, TCRN, CPEN
Kate Faranda
"I was an ER nurse at a community hospital for six years before I came to Stony Brook. One might think you’d get lost in the shuffle at a bigger hospital, but that just isn’t the case here. You still get that tight-knit, community feeling. We are a family. And I’ve been with this family for 10 years now. During that time, I went on maternity leave for a while and returned at the height of COVID. It was terrifying in general but then to be a new mom, as well, and to worry about bringing something home to your baby was just the worst. But when I walked into this hospital upon my return, there was a sense of comfort. It was neighbors helping neighbors. Everybody had each other’s backs regardless of what unit or department they belonged to. And that’s Stony Brook.
But it’s not just that community feeling that’s kept me here. There is so much that Stony Brook has to offer its employees. The biggest thing it had to offer me was the opportunity to learn and grow. And I’m STILL learning and growing. I started here in the Emergency Department. I did that for a little over six years. Then, I wanted change. But I didn’t need to leave Stony Brook for that. I had the opportunity to work in the Medical ICU. Then I ended up in the Neuro ICU, which is where I am now, and it’s a great fit for me.
Growing up, my mom always said I should be a nurse. And, of course, I would always blow it off. But one day after high school I was like…maybe I should go to nursing school. And here I am. I love my job. Taking care of patients is my calling. The best feeling is when somebody you’ve cared for gets better and you can join them and their family in rejoicing. It’s moments like that when I think of just how proud my mom would be of me today. She always knew this is what I would end up doing one day."
Kate Faranda, RN, BSN
Black History Month
“Black History Month is a time when people are paying attention to black stories, black issues, and black people. It shouldn’t be the only time, but right now is when we have peoples’ attention. Therefore, we feel this is a good time to feature Black Excellence in Medicine at Stony Brook. More specifically, highlighting the work of faculty in the Renaissance School of Medicine at Stony Brook University.
Unless a student has a class or rotation with a faculty member, they often won’t have the opportunity to get to know these people who are doing amazing work in their fields. And there is also a lack of awareness about the contributions of black people in medicine. That is why the Student National Medical Association (SNMA) at Stony Brook has decided to highlight black faculty this month in a daily student email. Some of these faculty members will also be featured on Stony Brook Medicine’s social media channels, as well. We hope that these efforts will do a number of things: create a way for students of color to see what faculty of color are doing and to be inspired by them and even motivated to reach out for mentorship and other opportunities; emphasize the importance of diversity in medicine; and ensure that students of color see themselves represented when looking at success.
Black Excellence in Medicine means seeing black people thriving in healthcare; dispelling the stereotypes that are often placed on us; doing more than what is typically expected of us; proving no challenge to be unsurmountable; and so much more.
Reflecting on the past is important but it’s not enough. We also need to look at the present in order to pave the way for a promising future.”
Adaora Ezike, MS1
Adaora has always had a passion for women’s health and wants to be able to provide culturally-competent sexual and reproductive health to women. She is particularly interested in addressing maternal mortality and access to quality healthcare both in the U.S. and in her home country, Nigeria.
Anecine Dalmeus, MS1
Anecine intends to help people who look her, not only as a physician, but also to set an example about what a black woman can achieve.
Chimdi Obinero, MS1
Chimdi would like to open his own practice one day, giving him the freedom to organize missions abroad, particularly for communities in Nigeria.
Jedan Phillips
"One of my primary motivators for going into academia was the opportunity to look at some of the experiences I had as a student and try to change them for others. It’s one thing to say that something shouldn’t have happened or been a certain way, but it’s entirely different when you can get involved in the medical education process and implement change. One way I can make an impact in this arena is through my involvement in SBHOME (Stony Brook Health Outreach and Medical Education). SBHOME is a pro bono clinic run by medical students and supervised by physicians. The clinic provides primary care to uninsured adults across Long Island at no cost. These efforts help underserved communities while making our students better healthcare providers. This experience teaches our students to be more aware of social determinants that might impact patient care. The experience also emphasizes the importance of understanding the communities we serve.
I also hope that as an educator and physician, students look at me and see somebody they can relate to. And that doesn’t just mean through race. It can also mean that someone comes from a similar background as my own. Seeing an individual in a position of power or success who you can relate to and understanding the path they took to get where they are can help provide a template for how to make your own success. My mother would always send me articles of prominent physicians of color. I would read about them and see these people in this space constantly achieving and doing great things. Something like that – seeing this representation - makes you feel confident in your ability to contribute, as well. It allows you to aspire to achieve. That’s what it did for me. And I hope I do that for others – not just in medicine, but in life."
Jedan Phillips, MD
Family Medicine
Medical Director, SBHOME
Allison McLarty
"Excellence in medicine is critically important. I believe that in America, there is sometimes this impression that what is produced by black people is not quite as good. Of course, there are exceptions, but that’s the problem – excellent black doctors are often considered exceptions. Frankly, I find this to be offensive. I was raised to be the best that I can be without consideration of the color of my skin. However, I suppose I’ve always felt this extra responsibility to excel because I am black to exemplify black excellence.
I think we are working towards a day when “excellence” does not need to be hyphenated by a race or ethnicity. I feel it’s part of my charge as a professional, teacher and mentor to emphasize the point that excellence is possible regardless of the color of one’s skin. So, to sum this up, I think black excellence is important, but I think excellence should not be defined by color.
We absorb our environment much more than we realize. What we see modeled before us imprints itself, therefore seeing one’s self represented really matters. For example, my mother was a working mom. She excelled in her career and was very well-respected. I saw her hard work and excellence while I was growing up, and it had a very powerful impact on me. When I became a cardiothoracic surgeon, there were few women, never mind black women, for me to emulate. But I had this image of a successful black female leader that I had observed throughout my life to guide me and that has been invaluable throughout my career. So I endorse the importance of having role models that look like us, even if not found in one’s specialty.
We are all standing on the shoulders of giants who came before us. It’s our responsibility to make sure we continue this important work for those coming after us."
Allison McLarty, MD
Surgical Director, Ventricular Assist Device Program
Associate Professor of Surgery, Renaissance School of Medicine at Stony Brook University
Jennifer McCoy
"For me, nursing is more than just working in healthcare. It’s about connecting with patients. Nobody wants to be admitted to the hospital. It’s difficult, particularly during times like the holidays. So, getting to be a light for patients is really what drew me to this profession, and honestly, it’s what keeps me here, as well. I originally wanted to work at Stony Brook because I loved that it was a teaching hospital. I wanted to learn as much as I could. Since being here, I’ve realized that the learning never stops. You can grow and advance your career here. You can even become the teacher or the mentor, which is something I really enjoy, as well. I recently joined unit-based council, which has been another incredible opportunity. We get together with nurses from other units and see what’s working best in other units and strategizing how to best implement different things around the hospital. I feel like I’m really making a difference here.
I find my work so very rewarding. I take something away from every shift that never ceases to make me feel so lucky to be a nurse. We are helping people every day. Special people – with their own incredible stories. And I just happen to work with the best team. Our unit is a family. So again, I just feel very lucky."
Jennifer McCoy, RN-BSN
(13N Neurology)
Caroline Smolkin
“My grandmother was a physician in the former Soviet Union. Although she never practiced in the United States, she was always a doctor in her heart and mind. So, I saw from an early age what it looked like to be a woman who people could look up to and rely on. That sparked my interest in wanting to help and advocate for people. As I continued to pursue the field of medicine, I realized general surgery is where I’m meant to be. I found it to be a very hands-on specialty where my extroverted personality would be most welcome. The range of cases I will be taking on throughout my career is exciting to me, as well. And I look forward to narrowing down which type of surgery I want to focus on in the future.
There aren’t as many female surgeons out there as one might think, and so I don’t take it lightly that I am pursuing a career in a historically male-dominated field. With that said, there happen to be a lot of incredible female surgeons here at Stony Brook. Throughout my rotations, I have worked with numerous female surgeons who have been advocates for women in medical school. It’s really empowering to be mentored by these surgeons who feel so deeply about lifting women up, and particularly women in medicine. I have taken what I have learned from them thus far and applied it to my own efforts in making a positive impact. Thinking about my grandmother, I know she is proud of the work I am doing, as well. She always knew I’d be a doctor.”
Caroline Smolkin
MS3, General Surgery
Stony Brook University
Soumya Mandava
“My interest in medicine started when I was five years old because of my pediatrician, Dr. Bhatia. She was loving, kind, highly knowledgeable, and able to share complex information in a way that even my young mind was able to comprehend. I will never forget the first time we went to see her. One of my sister’s braids had fallen out, and our doctor took the time to re-braid her hair. Who does that? A doctor who genuinely cares about her patients. My parents felt like their kids were in good hands, and I want to provide that same peace of mind for my patients. As I got older, I just knew I wanted to be part of this profession where I can make a difference and serve with compassion. My pediatrician was my first female role model in medicine, and she is one of my biggest advocates to this day. She even took a chance on me and let me shadow her, which is when I got to see, for the first time, that this profession was everything I hoped it would be.
I think one of the most important ways we, as women, can make a difference is by actively contributing to and being part of our communities. For me, it’s medicine. Remembering those who worked and sacrificed to build this foundation for us; ensuring we support and look out for everyone who walks beside us; and standing for and clearing the path for those who come after. I hope I make a difference by listening, being a voice and an ally, and by standing with my classmates and colleagues every day.”
Soumya Mandava, MS3
Interest in Anesthesiology
Stony Brook University
Regina DiBlasi
“Back when I first started at Stony Brook as a nurse intern in 1988, I thought I would only be here for a few years. I could not have been more wrong. It didn’t take long for me to discover that the nursing care here was second to none. Stony Brook was cutting edge even back then. It’s such an exciting and intellectual environment to work in – so much so that I don’t even mind my long commute.
I’ve always felt like I was born to be a nurse. I even used to help take care of my grandmother when I was a teenager. But to be in healthcare and to be a nurse, you have to be adaptable to change. And what’s so great is that Stony Brook is just as adaptable to your own personal changes, as well. If you want to learn and grow, you can do that here. If you want to explore different units and departments, you can do that too. And that’s exactly what I did. I was a SICU RN for a long time. Eventually, I was ready for change, so I transferred to outpatient surgical oncology in 2006. After three years there, I became an oncology-certified nurse (OCN), and then I became a nurse educator for the entire Cancer Center when they were in their old location. Fast forward to now, where I am currently the unit educator for the MART Multidisciplinary Clinic. I also recently earned my master’s degree in nursing education.
Lastly, I can’t go without mentioning the people here. I lead a really great staff, and I try to always give them the right tools and empower them to be able to practice at the highest level.”
Regina DiBlasi, RN, MSN-Ed, OCN
Nurse Educator-T&R III
Stony Brook Cancer Center
Multidisciplinary Oncology Clinic
Jennifer Burdish
“I consider myself to be an advocate for patients and for my staff. And I love what I do. I supervise the crisis prevention team, preventing and managing crisis situations throughout Stony Brook University Hospital. It’s great to not only be able to help patients, but staff, as well. Doing what we do allows other staff throughout the hospital to continue doing their jobs uninterrupted. Altogether, this leads to optimal care for our patients.
My team is amazing. Everybody always gives 110%, and each person brings something different to the table. We all come from different backgrounds and have had different life experiences, and we just complement each other really well. This is particularly important given what we do. Anything can trigger someone’s behavior, and sometimes it can be scary helping people through their worst behavioral crises. But we work as a team, supporting one another and always having the patient’s best interests in mind. And that leads to great outcomes. Our goal is always to help our patients to recover both physically and mentally."
Jennifer Burdish, MS.Ed, BCBA, LBA
Behavioral Health PMCS Coach
Stony Brook University Hospital
Department of Psychiatry
Helene V. Fall
“I’ve spent my entire career in community-based organizations. So, after I retired and we settled into our new home, I knew I wanted to volunteer. Stony Brook Eastern Long Island Hospital was an obvious choice for me. Having SBELIH nearby was very important for me and my husband because we knew having quality healthcare was going to be a significant part of our lives as we matured. Six weeks after we moved here and all the boxes were unpacked, I saw an ad in the local paper. I knew it was time for me to get involved. I started volunteering in the Opportunity Shop (thrift shop), and a few months later, I was asked to sit on the Eastern Long Island Hospital Auxiliary Executive Board. Fast forward ten years later to now, and I’m currently in my third term as Auxiliary President and remain an active in-Hospital volunteer, with 10,000 hours of volunteer service through the end of 2021.
I always aim to be heavily involved in my community, and the Auxiliary allows me to do that. The Auxiliary, which helped found the Hospital in 1905, remains a vital partner today providing 20,000 volunteers hours on average each year. We have donated close to $12 million dollars since our inception to assist the Hospital in providing critical services for our community. We consider ourselves community ambassadors for SBELIH, really. People even recognize me at the grocery store after work when I still have my volunteer smock on. We are highly identifiable and staples in the community.
I am so proud to be part of the Auxiliary, and I’m grateful for the affiliation with Stony Brook as it ensures our continued success. We have phenomenal people who work here and throughout the health system. It means a lot to belong to this community."
Helene V. Fall
President, SBELIH Auxiliary
Dawn Francisquini
“When I was younger, I had some personal family experiences at Stony Brook University Hospital. And those experiences helped take a very difficult time and make it honestly really positive. They were so impactful, in fact, that it’s what led me to want to go into medicine in the first place. And what’s more, I always wanted to be here at Stony Brook. It’s a special place for me. Stony Brook is where I had my first nursing job (2005). It was in general surgery. Over time, a lot of changes happened within my area, and the scope of patients we cared for started to expand. I became increasingly interested in working with kidney transplant patients. Working with them just gave me a different feeling. A special feeling. There’s nothing quite like seeing a patient before having a transplant and then literally watching as their new organ kicks in.
One day, there happened to be an opening for a transplant coordinator here, so I took a leap of faith. I just knew there was more I could do in this field. I became an outreach coordinator for the transplant program in 2012. And now I’m the administrative director, where I oversee all the daily operations of the transplant program, which includes both living donation and kidney transplantation. I’m also a certified transplant coordinator, so I am clinical, as well as administrative.
Nobody wants to be in the hospital. It’s anxiety provoking to say the least. And I believe the more supported a patient feels, the more successful their recovery will be. It’s the confidence that you give them as their healthcare providers and caretakers. I want our patients to know they can rely on us. I want them to feel safe, and I want them to know they are family. Every patient has a unique situation and their own story. And I make sure I know them all. I may be a healthcare administrator and a nurse, but I am human first. And my patients are human first. Simply put, we are in this together.
Dawn Francisquini, MSN, BS, RN, CCTC
Jerry Leigh
"I’ve been at Stony Brook for over 30 years now. I started as an officer and worked my way up to where I am now as the Director of Public Safety. On paper, the job is security. And although that is crucial, it’s more to us than just that. We don’t just sit in booths all day. We are out in the community building relationships and protecting the hospital and the university.
This type of role is in my blood. Fun fact: I was born in Scotland and came to the U.S. when I was six. My dad was in the military. We lived in Ocean Beach on Fire Island, where my dad was a police sergeant. His profession absolutely inspired my own. I grew up watching him work hard and save so many lives. So, I pretty much always knew I wanted to be in law enforcement.
In addition to what I do at Stony Brook, I’m also a volunteer firefighter. Along with many other first responders, I was on the ground in Manhattan during 9/11. That experience affected who I was both personally and professionally. I saw the hatred that came out of those devastating events, and I do my best to keep hatred like that out of this community – my community. I love working at Stony Brook. And I love what I do. We are a family here. I see people walk in and out of here experiencing both life and loss. Being able to be there for them in any case is the reason we do this."
Jerry Leigh
Director of Public Safety
SBU Office of Enterprise Risk Management
Associate Directors of Public Safety
Meet Joe Murrin, Dwayne Raye and Chris Seidensticker, Associate Directors of Public Safety here at Stony Brook Medicine.
Joe: Safety and security – it’s what we do. And keeping children safe in our facility is a priority. It’s my priority. In fact, I helped spearhead our infant protection system, so no child would be able to leave the hospital without a parent or guardian. Ultimately, we provide our patients and family members a safe and secure environment in our facility. When you walk through these doors, you are family. And we protect our family. And we all feel this way. I know this because I help to onboard new hires, as well. We train, set expectations, and make sure every single officer is ready for each and every day. The fact that I take on these extra responsibilities is a testament to how much I love my job. I am blessed to be here at Stony Brook.
Dwayne: I have a strong passion for critical thinking and strategy that is matched with a real desire to protect. Here at Stony Brook, I get to do it all. I work to identify potential risks or things that might make us vulnerable and then craft policies to prevent anything negative from happening. Education and communication are the key to success in security and healthcare, the more we teach and show our employees the safest way to work the better prepared we are for events as they arise. It’s about situational awareness. We need to give our staff the tools to operate autonomously but also effectively and carefully. My job is all about being proactive in a society that is predominantly reactive. And it’s all to keep the Stony Brook community safe.
Chris: Our job is to keep this community safe, and I think we do a great job, but we can always do more! I strive to make this a safer environment every single day. Part of my job is to evaluate our incident reports, and make strategic recommendations informed by my data analysis. This is so we can drill down, identify deficiencies and implement mitigation strategies across the Stony Brook Medicine Health System. I also have the opportunity to participate in the “Putting Safety First” program which provides opportunities to talk about global safety issues and receive feedback on how we can enhance the Public Safety program. I really enjoy what I do. Stony Brook is a second home to me, and my colleagues are like family. Working with them to protect our community is everything.
Marianne Bastian
"Like many who work at Stony Brook Medicine, my office is in Tech Park on Belle Mead. It’s a very busy road with a heavy Stony Brook presence – staff and patients alike. About four years ago, a goose was hit by a car and killed right in front of our building. It was very upsetting. As I was driving home later that day, I passed some lawn signs and it hit me. I came into work the next day, and with the help of my colleagues Anita and Donna, we created and printed signs to try to get people to slow down on Belle Mead. It was a real group effort. We needed to connect with property management, traffic safety, and the police department to make this happen. We even secured more speed patrolling in the area. And four years later, I do think it’s helped. We unfortunately still lose geese, but I feel like people have slowed down and are more cautious because of our efforts.
I’ve been at Stony Brook for nine years now, and I love what I do. I work in marketing and communications with some of the smartest, most hardworking professionals I know. We are responsible for messaging, both internally to staff and externally to the community, and that includes everything from COVID protocols and new hospital services to highlighting SBM’s pioneering research and programs. And we ensure the integrity of the Stony Brook Medicine brand. I think communication is what life is all about – sharing our ideas, thoughts, hopes and dreams with each other to hopefully ensure a more peaceful world. And that’s what I think these signs do. They communicate to the drivers that they are not the only ones on the road. We are a community-minded health system. And anything that affects our community matters, whether it be footed or feathered."
Marianne Bastian
Office of Marketing and Communication
Meghan Doelger
"I’m a nurse scientist at Stony Brook University Hospital. This is actually a new role nationwide. I’m going to help bridge the gap between research and practice for nurses at Stony Brook. On average, it takes about 17 years for research to be put into practice, so I’m here to expedite that process. When COVID first hit, I was in the middle of my doctoral project, and I ended up changing it to something more relevant. Since it was all hands on deck during the pandemic and people were just helping where they could, I created an educational program at Stony Brook for nurses who were being sent to the ICU for the first time. I went through the entire research process from designing the program to implementation, measurement of results and publication of the study. We had great results: the program significantly increased knowledge and confidence in the skills of the nurses. In a time when we were all in uncharted territory, I wanted to make sure that our most critical patients were being cared for by nurses who had the tools they needed to rise to the challenge. It was really rewarding to be successful in that goal.
The fact that this is a new role is really exciting to me. I like challenges, and I enjoy building things from the ground-up, making them my own and setting the tone for what’s to come. I want to make sure that Stony Brook Nursing is on the forefront of nursing science so that we can continue to elevate the care that we provide to our patients."
Meghan Doelger, DNP, RN, CCRN
Nurse Scientist
Pia York and John Marco Manzella
“As Concierge Supervisors, we are very fortunate to work with an amazing team of people. The Concierge staff bring lots of different skills to the table and are collaborative, supportive, flexible and exemplify teamwork. As Concierge staff, our goal as part of the Patient Experience team is to assist individuals with their needs. We are the first touch when people enter the facility, and we want to make sure we leave them with an overall therapeutic experience.
Our front desks are titled, “Information Desk,” but we are so much more than that. Whether we are walking someone to an elevator, assisting with a wheelchair, or helping them find their way, we want to leave people with an overall good feeling. We are active listeners, liaisons, de-escalators, facilitators, communicators, problem solvers and advocates. We understand people are not always here under the best of circumstances, and we empathize. Each and every one of us as human beings have, at some point, experienced some form of illness, loss or suffering. We keep this at the forefront of our minds and treat people the way we would want to be treated in their situation.
Though we are not clinical, we strive to provide a compassionate and caring approach. We hope to be remembered for being helpful and making someone’s hospital visit a positive experience. We always aim to make a difference and to be the difference."
Pia York
Concierge Supervisor
Stony Brook University Hospital
John Marco Manzella
Concierge Supervisor
Stony Brook University Hospital
Amy Karriker
"When patients come into the hospital, whether for illness or injury, many begin to ponder their own mortality. Whenever someone is confronted with this thought-provoking concept, often faith will come back up, if not already at the forefront of someone’s mind. Many people may not find themselves to be very religious but when they get sick or injured, faith has a tendency to appear. So, if we can help people come to a place of comfort or understanding, we have done our job. We may not be able to heal someone’s body, but we can help heal their spirit.
As Director of Spiritual Care, I have the privilege of leading a diverse team of professional chaplains to help provide compassionate care to patients, families and staff, which is the driving force behind our mission statement and the patient experience. Chaplaincy, like any other form of ministry, is considered a calling by God. I received my calling when I was a freshman in college. I wasn’t exactly sure of my direction, but I knew I was on the right track. I continued to pursue ministry in my education, which eventually brought me to seminary. One of the courses I had to take there was called Clinical Pastoral Education. I initially didn’t want to take this course because I strongly disliked everything about hospitals. I tried so hard to get out of it, but I was ultimately unsuccessful and had to take it. As soon as I did, everything clicked. I realized this was exactly what I was supposed to be doing. So, it was definitely divine intervention that I was unable to get out of that class.
I have been in chaplaincy for 30 years. I’ve worked in large teaching hospitals, children’s hospitals, rural hospitals, city hospitals, in the hospice setting, and so on. And I see myself in the hospital setting for the rest of my career. In fact, I see myself here at Stony Brook, specifically, for the duration. Stony Brook has everything anyone could ever ask for in a hospital. And with that comes a lot of opportunity for providing spiritual care to people. Chaplaincy typically struggles with career growth, but that’s not really the case at Stony Brook. I have the opportunity to grow here more than I ever have anywhere else. It’s exciting. Part of that growth was being able to bring a CPE program here. CPE is our clinical training, and it’s the first time Stony Brook has had this. It’s the only CPE program in Suffolk County and one of three on Long Island. We are very excited to see where this goes. And I am so looking forward to all of the good our spiritual care team will continue to do for our community. We grow in new ways every day as we continue to enhance the patient experience."
Amy Karriker, M.Div., BCC
Director of Spiritual Care
Jacqueline Coffey
"Back in nursing school, if someone had said I’d be working in Trauma one day, I would have run from the building and never looked back. It just wasn’t something I thought I’d ever be interested in. And yet here I am. As a Clinical Care Coordinator for Trauma Services, I do a million little things behind the scenes. I talk to patients and families; facilitate information between social workers, doctors and nurses; and pretty much make sure everybody has their piece of the puzzle that they need to save lives.
I respect this team of physicians here at Stony Brook so much. They are some of the best doctors in the game. I literally watch these heroes drop whatever they are doing and run to the Emergency Department when somebody needs them. It’s just incredible.
Every day is different in Trauma, and I love that. But working in this department can also be taxing on some. In addition to my work in Trauma, I’m also a Wellness Champion. We are a group of Stony Brook employees who make sure our teams are doing okay. If we see someone having a hard time, we take a moment to ask how they are really doing. This type of care for my peers really became a passion of mine during the COVID crisis. People were helping Trauma patients while working through their own personal trauma. It was a surreal time, and I just remember asking my colleagues how they were doing – for real. And the answers I would get were just very humbling. I decided this was something I needed to keep doing. We need to care for each other, as well as for our patients."
Jacqueline Coffey, RN
Clinical Care Coordinator for Trauma Services
Shari Hymes
"Stony Brook is a big part of who I am. I graduated from Stony Brook University back in ’84, and I’ve worked across all Stony Brook Hospitals. I know a lot of people, and we all work really well together and have each other’s backs. And I think this was illustrated and reinforced throughout the pandemic. It didn’t matter which Stony Brook facility you were part of. We all banded together and did what needed to be done. We were, and continue to be, one Stony Brook.
As respiratory therapists, we are there for the critically ill, as well as those with chronic illnesses. We are all encompassing. I think people really started to see our impact when the pandemic hit. A respiratory therapist is critical to any healthcare team. I’m very proud to be a respiratory therapist, and I’m proud of all my colleagues in this profession. I also have great supervisors who make sure their staff are taken care of and have what they need to perform at their very best. That’s integral for our success and for the well-being of our patients."
Shari Hymes ‘84
Respiratory Therapist
Denise Reilly
"I am a strong advocate for the patient. I grew up in hospitals, so I know firsthand that being in this type of setting can be overwhelming. In addition to the stressors from being here in the first place, most people don’t even understand the complicated medical terms and acronyms that are thrown at them. But it’s not about dumbing it down. It’s about making it real. It’s about creating an empathetic and personal experience and getting patients and families what they need, when they need it. This is a very important piece of what I do at Stony Brook.
I primarily work with the technology our patients engage with. Our patient portal is a great example of this. We are constantly enhancing this tech to make sure it’s exactly what our patients need. Whether they need to access test results, renew a prescription, message their doctor, or receive important updates from us, such as vaccine eligibility and availability, we want to make interacting with us as seamless and stress-free as possible. I am also very involved in our ambulatory strategy, as my background is in building and running ambulatory programs. I am part of a team that continues to work on uniform messaging and experiences across our organization. The goal is wherever our patients go within the Stony Brook system, there should be consistency.
I am also very involved with other technologies across the health system, as well, including cost accounting; ordering of clinical supplies; staff timekeeping system; and our health information exchange, which allows for a more comprehensive healthcare experience. For example, if you see a doctor at one of our outpatient facilities and then, on a separate occasion, go to one of our hospitals, your provider will have access to your information. In other words, you won’t need to bring your medical records from one place to another.
Stony Brook is on the cutting edge of providing patient care that is meaningful and technologically-advanced. I just feel very lucky to be part of all this in a place where the patient comes first."
Denise Reilly
Director, Patient Engaging Technologies, Health Information Exchange, and Ambulatory Strategy
Stony Brook Medicine
Lynne Alba
"As Director of Talent Acquisition, I oversee the hiring and acquisition of talent for Stony Brook University Hospital - everything from hospital attendants, nurses to our most senior leadership positions. This job is so special to me because not only are we bringing meaningful jobs to deserving candidates, but we are also bringing talented, hardworking people to Stony Brook. We really provide a service that enhances patient care and the patient experience by making sure we have the right people in the right places.
Finding and attracting healthcare talent across Long Island and New York State has always been critical. But we make it a point to stay on top of trends and embrace changes in the preferences of people – our applicants. Candidate preferences and behavior evolve and change based on the time and space that we are in. For example, a lot of people prefer to watch content instead of reading it. People won’t watch a long video on social media, but if I can get my point across in a minute or less, they might watch to the end. This brings me to my TikTok presence, which is really something that happened rather organically and has been received quite well. It was definitely out of my comfort zone, but it’s working. We are filling jobs, getting referrals, and people are telling me they are learning things. I see this as an opportunity to provide value and share tips and tricks with candidates and fellow recruiters, and I am so glad that it’s working.
Aside from being a “Talent Acquisition Influencer,” I am also a leader. And I have to say, my team is just incredible. They are hardworking, creative, and fearless when it comes to trying new approaches to recruitment. I think we have all learned over the years that although this job can be very strategic, creativity is ultimately the strategy. And I appreciate the chance for all of us to be creative. My entire team is made up of heroes – heroes who recruit heroes."
Lynne Alba
Director of Talent Acquisition
Stony Brook University Hospital
Marquise Soto
"Being Black in medicine is an honor and privilege. We are an underrepresented but essential component of a diverse and growing medical field. I believe as an Afro-Latino in medicine, I have a responsibility to be a role model for minority students interested in pursuing careers in medicine; to be an inspiration to the dedicated group of practicing Black physicians; and to provide a pathway to restoring my community's faith in the healthcare system.
Black Men In White Coats™ is an organization committed to battling our nation's current health care crisis of having a shortage of Black male physicians. A Black Men in White Coats™ chapter is vital here at Stony Brook University. With our institution’s resources and commitment to diversity, I am positive we can do more to impact and increase the representation of Black male medical students and physicians.
#BlackHistoryMonth is such an important time for reflection, inspiration and motivation. As Black people, it is a tribute to how far we have come and all we have done despite the many challenges we have faced. It serves as inspiration and motivation for us to see the successes of our community. It serves as a reminder for all that our impact cannot be silenced and that allyship is such an important part of effecting positive social change. It is not enough to recognize our accomplishments. We must learn from our failures and do better by not confining Black history to a month. Black history is every day, and you can always do something to amplify someone's voice, celebrate a friend's accomplishments, apologize for an insensitive comment, revise your previously-held notions, and choose to encourage and uplift others. It is the key to not making this a sentiment for the month but rather a lifestyle change. Having an active Black Men in White Coats™ chapter is an example of this – an effort that extends beyond a single month. An acknowledgment that there is still work to be done. And a commitment to diversity."
Marquise Soto ’25 (MS2)
Inaugural President and Co-Founder
Black Men in White Coats™ affiliate chapter at Renaissance School of Medicine at Stony Brook University
Chimdindu Obinero
"For me, being Black in medicine has been very multifaceted. My experience is not limited to this moment in time but also involves all of the experiences that lead up to this point. Those experiences molded me into the person I am today, and when I look back at them, I feel stronger. I think of the person who experienced institutionalized racism in healthcare and academia and still decided to pursue medicine. I think of the person who felt the joy of speaking with black youth who want to be in my shoes one day. My journey has been filled with ups and downs, but reflecting on how far I have come in spite of the obstacles is always empowering.
Black Men In White Coats is an organization of physicians and medical students who seek to address the declining number of black males pursuing medicine as a career. We collaborate with local schools and community leaders to host panels, workshops, community fairs, and other events aimed at bolstering interest in the field. We also aim to act as role models for young black boys who wish to one day work in healthcare. We were lucky to have the privilege of establishing the first Chapter of Black Men in White Coats in our regional area of New York. When the black boys of today become the medical students of tomorrow, we want to make sure they have the Renaissance School of Medicine at Stony Brook University on their application list.
#BlackHistoryMonth gives us a chance to celebrate the experiences and contributions of black people in America. Sometimes it is so easy to get caught up on how far we have to go before we achieve true equality, that we can forget how far we have come. We need this month to celebrate and reflect on the past. However, as the month comes to a close, we can use this period of reflection as an opportunity to apply the lessons we have learned to our future endeavors. I want people to understand that obstacles can be overcome. I know I have been lucky in many ways, including the support I have received from those who have always wanted me to succeed. So, I want those who come after me to know that I am in their corner cheering them on. I want them to succeed. And I hope the work I am doing now with Black Men in White Coats contributes to the success of our future Black physicians."
Chimdindu Obinero ’25 (MS2)
Inaugural Vice President and Co-Founder
Black Men in White Coats™ affiliate chapter at Renaissance School of Medicine at Stony Brook University
Stephanie Ratzke
"I’ve been a pediatric nurse for almost 10 years now. As such, I care for children and support their families on their worst days. I love being a pediatric nurse. There is a special joy you get in working with children, and the sense of value you feel when you see them get better and their families relieved is just unmatched. I also value what I do even more now as a parent, myself. If a child is ill with something we think might be minor, it’s still a parent’s worst day. So, to provide families with support, in addition to caring for their children, is very fulfilling to me.
Since May, I’ve been the nurse educator in Pediatrics Acute and Pediatric Hematology/Oncology, and so recently I’ve been more heavily focused on encouraging our nurses to become certified. Personally, I wanted to become certified to better myself and the care I provide to my patients. Certification helps me to maintain my confidence in the work I do and also keeps me actively involved in the newest and best practices that help me to provide the best possible care to my patients. It’s important to invest in yourself. And Stony Brook is a great place to be for that. We want each other to grow and excel. We are all experts in our respective fields, and certification is another way to let everyone know. It’s a way to give not only yourself confidence but to give your patients and their families confidence in the care they are receiving, as well. It holds meaningful weight."
Stephanie Ratzke, RN, BSN, CPN
Nurse Educator
Pediatrics Acute and Pediatric Hematology/Oncology
Daphne Perry
"Alzheimer’s does not discriminate. It transcends the boundaries of race, sex, ethnicity and religion. And it kills more individuals than breast cancer and prostate cancer combined. It’s the most common form of dementia in older people and the sixth-leading cause of death in the United States. As Program Director for the Stony Brook Center of Excellence for Alzheimer’s Disease, I empower my team to meet our program’s goals and objectives of ensuring individuals affected by Alzheimer’s Disease and their families are well aware of available services, supports and resources that will help them maintain their quality of life for as long as possible. Our program is the only one of its kind on Long Island, established by New York State, to assist providers with making a dementia diagnosis; to help those providers with technical support; and to increase the awareness of providers, healthcare professionals, healthcare students, and the community at large about Alzheimer’s Disease. Education is power. I encourage people to be their number one health advocate and to listen to their bodies. If your memory isn’t quite right, get it checked.
In addition to my work with Stony Brook, I also write stories for children. Kids have a vivid imagination. They are impressionable, fearless, innocent, and they are open for adventure. When I was a child, my parents read to me. And when I became a parent, I read to my children. And then I began to make up my own stories, and they loved it. Then I started thinking, “I’m pretty good at this.” I’ve always enjoyed reading. It allows us to be transported from our world to another. And between the pages of a book, we know we can become immersed in the lives of fictional characters. We can learn about different cultures; children can learn new words and phrases; and we can all experience a range of emotions and acquire knowledge. When I was a child, I’d go to the library, and I’d look for books that had characters who looked like me on the cover. Those books were virtually nonexistent in my hometown library. My mom wrote a book for my daughter when she was born, and I read it and was totally inspired by it. I said, “Wow, I can do that.” Then, when my son was born, I took a leave from work and decided to do something that I enjoyed, which was write stories. So, I’ve written many stories, and now I’m in the process of publishing them. ‘ABCs of Love' was the first book that I wrote. Three weeks after it was released, it was number one on Amazon’s Hot New Releases in the Early Childhood Education category! My second book, My Very Busy Day, was just released on Amazon this past December.
As I’m getting older, I see the benefits of intergenerational connections between young children and older adults. My stories look at the world through the eyes of children who are innocent, adventurous and fearless. And some of my best friends who are in their 80s and 90s read my books and say they take them back to a time when they were carefree kids just enjoying life. It sparks a memory for them and puts a smile on their face. I also find that older people are happy when they share wisdom and experiences with children, and children are really receptive to learning. So, there’s a formative bond that happens. And one of the goals in our program here at Stony Brook is education. I actually think we should be teaching kids as young as middle schoolers about signs of Alzheimer’s. Oftentimes, grandparents serve as caregivers for their grandchildren. And these children need to be familiar with unusual behaviors so when they see them, they can say something about it."
Daphne Perry
Program Director
Stony Brook Center of Excellence for Alzheimer’s Disease
Lisa Sampson
"When a patient comes to us for an MRI or any other type of scan, they typically want results fast so they can be treated more quickly by our surgeons. That’s where I come in. I do all the authorizations for diagnostic imaging. And the reason why I like to do things quickly is because if that was me or someone in my family, I’d want answers. So I do everything in my power to get things done same day in order to make the experience as stress-free as possible for our patients. Who wants to get an MRI on a Friday and not have any answers until the following week? Nobody. I’ve been there, and I never want others to experience that. I think the best way to describe how I operate is that I do my job, and I do it with a conscience.
Some might wonder how I could possibly enjoy doing what I do – being behind the scenes, working with insurance companies and doing a lot of administrative work. The truth is – I LOVE my job. I really do. I love a challenge, and I love helping people. I’ve also been working in orthopedics for 37 years. Orthopedists are like the carpenters of the skeletal system, and it just really interests me. And I also like the people I work with. You have to have fun while you’re at work. I feel bad for people who don’t. My colleagues are like my second family. I just feel very good about myself while I’m at work. It lifts me up. Stony Brook is a family. We work with family, and we take care of family."
Lisa Sampson
Senior Administrative Assistant
Stony Brook Orthopaedic Associates
Chuck Mikell, MD
"Clinically, I’m focused on the brain. I treat chronic conditions such as #Parkinsons and #epilepsy with functional #neurosurgery, which focuses on restoring neurological function and quality of life to people with movement-related disorders that otherwise interrupt their day-to-day function or abilities. I’m also the co-director of the Neuro-Oncology Center, where I focus on malignant (cancerous) brain tumors. On the research side, I’m really interested in brain injury and the underlying processes that allow us to wake up and recover consciousness after a serious brain injury. I love my work. People come to me with serious problems, and my goal is to have them walk away with the ability to live life a lot fuller than they were previously able to. I can help patients move around more easily or need fewer medications. And for things like brain cancer, we’ve really moved the needle. #BrainCancer used to be an overwhelmingly bad prognosis. And although it still is, we have more and more patients who are doing well and living a lot longer.
Outside of my work at #StonyBrook, I also compete in #Strongman competitions. I’ve been doing them for about 10 years. I first got into it when I was a resident, but I’ve stuck with it since then. I enjoy loading and carrying heavy things like stones, logs, and kegs. Deadlift is my best event – I compete as a lightweight, and I came in first in the 181 lbs. weight class at New York's Strongest Man this year. I'm now getting ready for nationals in Denver in 2024.
Strongman has actually informed what I think of as a prerequisite for a fulfilling life. When you are older, you want to be able to carry your grandchildren or carry luggage through an airport. Carries are fundamentally core movements in Strongman and in everyday life. I try to emphasize with my patients that I encourage weight and resistance training, cardio and so on. I think fitness is a way for people to keep moving for as long as they can. And Strongman is a way for me to do the same – to keep living life and to be in shape so I can continue to help patients for as long as possible."
Chuck Mikell, MD
Neurosurgeon
Kathleen Logsdon Carrozza, MS, RD
"My primary focus is to make sure patients get a beautiful, hot meal that is appropriate for their diet, and that it’s delivered with a smile. I’ve seen firsthand how eating well can be critical for healing and recovery and that’s why I got into the field of nutrition. Some of our most important and memorable moments in life usually involve food. Sometimes patients in the hospital feel the only thing that they can control is what they eat, and it’s something I felt strongly about addressing.
When I was looking for ways to improve patient meal service, I saw a demonstration of new software, and I described it to our team. It wasn’t difficult to get everybody on board because Stony Brook is very forward-thinking; we really embrace innovation here. The more I talked about it with our team, the more excited everyone was to make this project a success! We had support from the administration, IT jumped right in, and our patient food service team was up for the challenge. Two Stony Brook University student interns also did a phenomenal job working with our culinary staff to photograph every item on the menu. I want patients to know that when they are ordering, they are not looking at stock photos - it’s real food from our kitchen. In order to educate the patients about the app, Alexandra Bush, our Nutrition Software System Administrator, has been going to the units to demonstrate the program and provide training.
So, fast forward to today, we have introduced our new mobile app that patients can use to order meals with their dietary restrictions in mind. Families can even order for their loved ones and schedule meals from outside the hospital. It’s a complement to the other existing ways that patients can order food. It helps with efficiency and improves the overall patient experience. Feedback on this app has been very positive thus far. It gives patients a sense of control. They are doing something that many of them are already familiar with.
I’m so proud of everybody involved with this project. They all rose to the occasion, they could understand the benefits and they just wanted to see it succeed. It’s a great feeling to watch something you are passionate about come to fruition. I even had the opportunity to try it as a patient recently; it worked great! It’s just like any other food ordering app you use at home. It makes things easy!"
Kathleen Logsdon Carrozza, MS, RD
Assistant Director of Food and Retail Services
Stony Brook University Hospital
Tauhid Mahmud, MD, MPH
"As residents, we have a unique perspective in medicine. Usually, we’re amongst the earliest adopters of new tech like generative artificial intelligence. And the thing is – patients are also experiencing and using these things, and they have questions about how it will impact them and their care. Residents can offer insights on this from the beginning.
This is actually my second residency program. I completed training in Family Medicine where I would often have patients share stories of how they couldn’t afford the insulin I prescribed or how dangerous it was to simply go for walks in their neighborhood. I realized I wanted to try to address the systemic problems affecting my patients’ health. Preventive Medicine allows me to do just that on a broader scale.
I am very fortunate to train at Stony Brook, where our program director embodies the ideal mentor – caring, dedicated to our growth, and invested in ensuring a fulfilling, productive residency. People here lift one another up and support each other’s development and success."
Tauhid Mahmud, MD, MPH
PGY-2, Preventive Medicine
Associate Editor, American Journal of Preventive Medicine (AJPM) Focus
Andre Demosthene and Victor Alonzo
"As biomedical engineers, it’s our job to make sure all medical equipment here at Stony Brook University Hospital is properly serviced and is being utilized in a safe manner. We operate with two things in mind: patient safety and customer service. It is a privilege to work here and to serve our community. We get to use our unique skill sets to make a difference in the lives of our patients, and we get to see the positive impact that we make, which is truly special and something we don’t take for granted.
Andre: One of the biggest highlights of my career thus far is when my wife and I were on the receiving end of the work my colleagues and I do. My two youngest children were born at Stony Brook, and to see familiar faces and equipment I quite literally worked on aiding in the birth of my children was just incredible.
Victor: All three of my daughters were born here. In fact, my whole family comes to this hospital. My dad was here for a while, and when I first started here, I was able to track down a nurse who cared for him, and I got to tell him how much he meant to my family. This place has always meant a lot to us.
Stony Brook University Hospital is an incredible place to work. It’s bigger than just a job. It’s a community. It’s family. There are so many opportunities to grow in your career here. We are both examples of that, and we are truly humbled to be in the positions that we are in. And the biomedical engineering department here is a special group within a special place. We accept this nomination of "Healthcare Heroes" on behalf of our entire department. They are the miracle workers here who keep things running so our healthcare workers can treat and care for our patients."
Andre Demosthene
Service Manager, Biomedical Engineering Department
Stony Brook University Hospital
Victor Alonzo
Director, Biomedical Engineering Department
Stony Brook University Hospital
Chander Sadasivan, PhD
"When I entered college, I originally had my sights set on mechanical engineering. One day, while flipping through an encyclopedia in the university library, I saw an entry for a flagellum, a thin, tail-like structure that bacteria and other microorganisms use to swim. I was stunned to see the complexity of this mechanism that nature had built. That was my ah-ha moment. I admit, I couldn’t foresee at age 19 how far the application of my engineering skills would take me in solving biological or medical problems through complex model design. I just knew that biomedical engineering might be a better fit for me. At the time, I received a lot of push back from friends and family back in India. They had been supportive of mechanical engineering as a career path, but the field of biomedical engineering was in its infancy, and they didn’t think a career in that field would go anywhere. Some even told me my career would be wasted. But I’ve learned in life that when you really want to accomplish something, you have to tune out even the most well-meaning naysayers and follow your instincts. So, I pushed forward, and I’m glad I did.
My research at Stony Brook is on interventional radiology medical devices. These are image guided devices using modalities such as fluoroscopy, ultrasound, computed tomography (CT) and magnetic resonance imaging (MRI) that physicians use to diagnose and treat patients. My focus is on neuro brain interventional surgery. I study blood flow dynamics in the brain, which is another way of saying that I study the movement of blood through the vessels from the arteries and capillaries and then into the veins of the brain. Because no two patients’ blood vessel anatomy and flow dynamics are the same, it can be tricky to select the correct device, guide it through the complex anatomy, and implant it at the right location. I custom-build replicas of a patient’s blood vessels by 3D printing their CT scans so that our surgeons can test out plans of treatment for each individual patient whose vessels are more complex. My lab has a high-end 3D printer to process this task. Using this approach, by the time a patient is in the OR, the surgeon knows exactly what route to take because it’s already been tested in that patient’s replica. No time is wasted. This work also helps educate the patient’s family — in a visual manner — about what the treatment plan will entail. It’s a great way to help manage expectations and alleviate fears of the unknown.
I had an aunt who suffered a ruptured brain aneurysm years ago, back when I was in grad school. This was devastating to my family. I keep wishing I could go back in time and do more for her. This lingers in the back of my mind throughout my work when replicating blood vessel abnormalities such as aneurysms to help patients today.
The Cerebrovascular Center for Research that I lead is also used to educate and train residents and other clinicians on procedures. There are always sounds of hammers and drills in the lab as students at all levels build different benchtop systems to test the replicas. They learn from me, and I learn from them. My students teach me how to mentor better every day. I feel very lucky to be working with these students and colleagues and with incredible physicians who are leaders in their respective fields. Beyond the Department of Neurosurgery, I collaborate with many other departments across Stony Brook – Vascular Surgery, the School of Dental Medicine, Mechanical Engineering, Materials Science and Chemical Engineering, Applied Mathematics and Computer Science to name a few. It’s incredible to see the many different applications of the work we do.
This work is very rewarding. For many researchers, years can go by before they see the fruits of their labor. My research is for immediate care, and it leads directly to better patient outcomes.
If you were to ask my family and friends today, what they think about my chosen profession, they’d probably say, “Chander, don’t say I told you so. We know now that you were right.” I know they’re very proud of me. They see what a difference my work makes in the lives of so many others."
Chander Sadasivan, PhD
Director
Cerebrovascular Center for Research
Chiagoziem Okolo, MS1
"Black History Month is a time to celebrate the numerous black achievements throughout the years. It’s a single month – the shortest of the year. But that just means we have more time in the year to create history. One way the Renaissance School of Medicine is doing that is through an organization called Black Men In White Coats (BMWC). The Stony Brook University Chapter of BMWC was formed last year by medical students. The main issue we tackle is the steep decline that we’ve seen in the presence of black male physicians over the years. In the last 80 years, the percentage of black male physicians in the medical field has only gone down. As the Director of Mentoring, I believe it’s important that our organization serves as a foundation for people like us who want to pursue a career in medicine. BMWC serves as a resource for them. Considering that black men make up a very small percentage of the field, we would like to lend a shoulder for others to stand on so we can eventually form a proportion of doctors that is representative of the communities we serve. We accomplish these goals through community outreach, mentoring, and providing opportunities for the future of medicine to gain skills and credentials that will help them become history-makers by the end of their medical pursuits.
In addition to my involvement in BMWC, I’m also a recipient of the WB Turner Fellowship that rewards individuals that have a similar background to WB Turner and who are committed to community service, civil justice, and academic excellence. I don’t take this opportunity lightly, as it is very helpful for students like me who have a difficult time paying for housing and putting myself through medical school. It allows me and others like me to be able to further our education and focus on what really matters: Making a difference.
It’s important to celebrate Black History Month because a lot of black achievements tend to get overshadowed. So, this month is an opportunity to make sure that doesn’t happen. It’s a chance to give credit where credit is due and to recognize and celebrate the real McCoy’s – the trailblazers, the truth seekers, the real deals."
Chiagoziem Okolo, MS1
Renaissance School of Medicine at Stony Brook University
Director of Mentoring, Black Men in White Coats, SBU Chapter
Erkan Arklan
"We work from roof to basement here in Housekeeping. But the most meaningful part for me is when I clean a patient room after discharge and before another patient is admitted. I clean each room as if the next patient coming in is somebody in my own family. Because that’s just it – the next person being admitted IS somebody’s loved one. I care about everybody. And I really see us here in Housekeeping as playing a critical role in the patient experience.
Stony Brook Eastern Long Island Hospital is a special place, and it’s not just because it’s so peaceful looking out at the water before walking into work! The people here are amazing. We are a family – literally. My wife works here, as well, in Dietary. We love seeing each other at work. And leadership is so supportive. My supervisor is the best manager I have ever had, and it doesn’t stop there. Our leader, Paul Connor, is equally amazing. Everybody is so nice. We are a tight-knit community, both inside and outside of the hospital. People sometimes call me the mayor because I know everybody! And I wouldn’t have it any other way. I’m in it for the long haul here at Stony Brook. It’s my place."
Erkan Arklan
Housekeeping
Stony Brook Eastern Long Island Hospital
Jedan Phillips, MD
Black History Month is about the past, present and future. History is made every day, and the students and providers at SB HOME (Stony Brook Health Outreach and Medical Education Clinic), including Jedan Phillips, MD, are part of that history as they continue to address healthcare disparities and serve vulnerable populations on Long Island
"I grew up in a community that was vulnerable due to limited access to quality medical care. It made me aware of what I did not have. Still, I was able to push through and succeed. It instilled in me the fire to do what I do now. Being the eldest of six, I also grew up with the inclination to work hard, open doors and hold those doors open for others. It’s become my passion, and I feel very fortunate that I get to do this every day with SB Home, where we provide pro bono medical care to the uninsured adults in the communities we serve.
SB HOME came to be when we started to see news around uninsured and immigrant populations on Long Island. Students at the Renaissance School of Medicine at Stony Brook University wanted to help address this problem. This work has not only helped our communities, but it has prepared students for their own professional pursuits, giving them experience in community outreach and showing them just how big of a role social determinants of health and disparities play in healthcare.
There are many levels of vulnerability, including but not limited to lack of access to quality medical care, literacy challenges, housing and food insecurity. While this is not solely a problem in black communities across Long Island, one of the biggest identifiers for a vulnerable population in Suffolk County is zip code – and those zip codes do tend to be black and brown communities.
We are helping people. We are educating and training providers to have a strong awareness as they get to know the communities they will serve."
Jedan Phillips, MD
Medical Director and Founding Faculty Member
SB Home
Keith J. Breglio, MD
"When I was in high school, my cousin was in a terrible car accident. For three months, she was in a coma in the pediatric ICU. I would visit her as often as I could. At that young age, I remember being comfortable in that setting. I was amazed witnessing the care she received. I realized during that time that being a doctor and caring for someone like her was something that I could do, and wanted to do. From then on, I focused on becoming a doctor. My cousin eventually recovered and I know she is going to read this and laugh. I can hear her saying "You are still using that story after 30 years? You owe me!"
Working in pediatrics has allowed me to care for a population of patients at a critical point in their lives, specifically their growth and development through childhood. As a Pediatric Gastroenterologist, I am able to care for these children, incorporating various diagnostic and therapeutic procedures as part of their treatment, which is something I really enjoy. Oftentimes in my specialty, I am lucky to follow my patients for months to many years. I see many of my patients as they grow well into their college years, which is very special to be a part of. It is a privilege to have the trust of the family to treat their child, and as a parent myself, I take that very seriously. I care very deeply for each of my patients, and I approach each one with compassion. I make a point to try and bond with each child on their level and hope that my bedside manner has made the kids, and their parents, feel at ease.
Stony Brook Children's is an incredible place to work because the focus is truly on the entire well-being of the child. Hospitals can be intimidating for kids and parents alike. That is where Stony Brook Children’s Hospital sets itself apart. In addition to the top tier medical care families here will receive, our amazing staff, including a wonderful child life program, dedicate their lives to make the experience for these children as pleasant as possible.
I have always prided myself on the way I take care of my patients. Being at an institution like Stony Brook allows my colleagues and I to provide the best care possible, to a tremendous population of children with complicated diseases, while striving to help these children focus on being a kid and not their disease. I feel very fortunate to work at an institution like Stony Brook that supports us in this noble endeavor."
Keith J. Breglio, MD
Director, Pediatric Endoscopy
Division of Pediatric Gastroenterology and Nutrition
Stony Brook Children's Hospital
Stony Brook University Hospital
Lisa Marie Gonzalez
"“ When someone asks me what I do for a living, I say I’m a pastry chef. They ask me, “ Where?” I say at Stony Brook University Hospital! Typically, their response is, “ WHAT?” Not many people know you can order cakes at the hospital. It’s such an element of surprise. “ Where’d you get that cake?” “ At Stony Brook!” I love it. I’m so proud to be here."
I’ve been baking for almost 20 years, and I’ve been baking at Stony Brook since 2017. We are a team of two here in the bakery. Kevin and I are a great team. We get creative and just work so well together. Having a partner is really empowering. We lift each other up. We bake for patients and for retail (cafeteria). We bake for doctors’ offices and any and every part of the hospital. And if you want to send a special treat to someone, we’ve got you covered.
It brings me such joy to be able to treat our patients and their families. And to put a smile on the faces of our healthcare heroes. People get joy from going to a bakery and ordering something for someone but I’m the one who gets to bake it, and that’s quite meaningful to me. We bake for YOU. If you have specific nutritional needs, dietary restrictions or allergies, we will bake something just for you – and it will taste amazing. I love when people say they can’t believe there’s no sugar in something we’ve baked! It’s an art and a science, and the end goal is always that whatever we bake tastes good and brings joy.
In addition to this work being my passion, I also love the growth at Stony Brook University Hospital. There are so many opportunities to grow and advance here. Change can be scary, but it’s also exciting. And I’m happy to be part of it here in my own way."
BONUS QUESTION: What’s your all-time favorite dessert? “ Personally, my favorite cake is a strawberry shortcake – but with a twist. I put strawberries AROUND the cake!”
Lisa Marie Gonzalez
Lead Baker at Stony Brook University Hospital
Award-Winning Pastry Chef
Meg Stern, MS, CPXP
"My first job out of college was in oncology, and that had a profound impact on my entire understanding of what it means to be human. I saw suffering, pain and uncertainty, but I also saw the power of compassion and connection and how that can impact peoples’ care experiences and lives. Seeing this – feeling this – that’s why I ended up pursuing the field of patient experience.
I feel so lucky to be part of an incredible team here at Stony Brook Medicine, and I wouldn't be where I am today without the immense support and encouragement from my leadership and colleagues. I work across all our hospitals and share our patient experience strategy, which is rooted in compassionate, connected care. And I also have the honor and privilege of hearing from caregivers and better understanding why they do what they do. I leave work every single day inspired by our healthcare workers, patients, and their loved ones. I get to witness and be part of the positive impact that Stony Brook has on our community. This is truly a one-of-a-kind organization. I would know! I have moved over 12 times, back and forth across the country, and I have never found a place quite like Stony Brook that is so impressive and yet is so community oriented. I feel very proud to work here.
Although I always believed in Compassionate, Connected Care, it wasn’t until I was a patient here, myself, that I could personally feel the profound impact it has on a patient. I chose to receive my prenatal care and deliver here at Stony Brook University Hospital. The connections I made with the staff here as a patient, myself, are something I will hold onto forever. They made me, my babies, and my partner feel so special, protected and cared for. They truly embodied compassion while providing the best possible care in a situation where I was rather uncertain. I will never forget them. And to be in a position at work where I can help give recognition to our caregivers by amplifying the voices of our patients is very special.
I feel so lucky every single day that I get to come to work at Stony Brook Medicine. Everybody that works here has a real passion for helping people. I truly believe working in healthcare is the most noble of professions, and I am so humbled and grateful to work with such incredible people."
Meg Stern, MS, CPXP
Patient Experience Educator
Stony Brook Medicine
Valmore Suprenant, MD
"My journey to healthcare was an interesting one. I started out in advertising and then at a software company in DC. I was riding my bike one day (something I love doing – it's how I beat the traffic in Southampton!), when I got to the top of a hill. I just stood there, looking out on Northern DC, and I had a moment of self-reflection. I just said to myself, “ I have got to do something, or life is going to pass me by.” I was 33 at the time, and I decided that the “ something” I needed to at least try was pre-med. I ended up really enjoying it, so I stuck with it. I got into medical school at 40 and ended up finding myself working with two vascular surgeons who changed my life. These two attendings were constantly operating, but their work ethic wasn’t limited to their work in the OR. No job was too small for them. If the floor needed to be mopped so an OR could be turned over for another patient and nobody was around to do it, they would. They always did what needed to be done, and it was invigorating to work with them. They showed me the type of doctor I wanted to be.
Fast forward to today – I'm an interventional radiologist, and I do a variety of procedures ranging from the small to the not-so-small. We place ports and venous access devices for patients undergoing chemotherapy, embolization procedures for different forms of cancer, abscess drainage, kidney stone removal, and much more. And a lot of what we do boils down to this: we save surgeons and patients from major operations. If we can control a bleed, that spares an open vascular surgical procedure. If we place an abscess drain, that keeps a patient out of the operating room for a surgical washout. One day, recently, I was about to head home when I was abruptly told, “ Don't go anywhere! We need you.” A patient had a c-section and the OBGYN found their left uterine artery had been transected, and they were not able to stop the bleeding. The team took the patient from Labor & Delivery to an operating room, and we began right away. We navigated to the transected artery, and as soon as I injected contrast, it was obvious there was a significant amount of bleeding. From inside a small catheter, we took a micro catheter and navigated into the uterine artery and placed two coils, immediately stopping the bleed. I have to say, the ability of the staff at Stony Brook Southampton Hospital to mobilize this patient and transport them quickly and safely to the OR was impressive, to say the least. The staff here really, truly care about our patients, and they have the skill and talent to do it effectively.
Something I ’d really like to leave people with is that it’s so important to not let your work, regardless of what it is, consume you. No matter how much you love your job, you don't want to get burned out. Adopt healthy habits. Find hobbies. Ride a bike. Play the drums. Balance is critical. It’s funny – I do play the drums, and part of playing this instrument is that you want to develop your weaker hand to play effectively. In my case, it’s my left hand. So, through playing the drums, I’m more coordinated and versatile, and I’ve developed a level of ambidexterity, which has helped me in my medical career. An OR can be set up in any way, and I can adapt and work around things.
This may sound corny, but not a day goes by where you don’t do something in this field. And I mean really do something – something meaningful. It can be the littlest thing like taking out a drain. Something that may not be critical but nobody likes having a drain in their kidney. So being able to give somebody relief like that is a great feeling. And then you have the more critical cases like the uterine artery embolization, where you are saving a life. And all of this – the big and the small – it keeps me coming back every day."
Valmore Suprenant, MD
Interventional Radiologist
Stony Brook University Hospital
Stony Brook Southampton Hospital